-
 Minnesota
MinnesotaMayo Clinic Health Letter: Highlights from the March 2015 Issue
ROCHESTER, Minn. ― Here are highlights from the March issue of Mayo Clinic Health Letter. You may cite this publication as often as you wish. Reprinting is allowed for a fee. Mayo Clinic Health Letter attribution is required. Include the following subscription information as your editorial policies permit: Visit http://healthletter.mayoclinic.com/ or call toll-free for subscription information, 1-800-333-9037, extension 9771. Full newsletter text: Mayo Clinic Health Letter March 2015 (for journalists only).
Alternate medications to manage chronic pain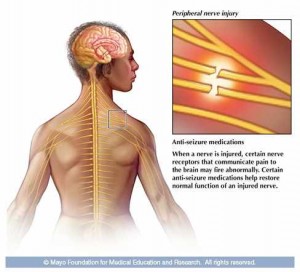
Pain medications might not work well for chronic pain ― pain that doesn’t go away with time. The March issue of Mayo Clinic Health Letter covers other types of medications and strategies to consider as part of long-term pain management.
Deciding on potential drug therapy for chronic pain usually involves analysis of the cause or causes of pain and knowing which type of drugs may be beneficial. Pain medications typically work well for pain resulting from headache, an injury or surgery. These same medications can lose their effectiveness over time, and some may even make pain worse or cause unacceptable side effects. Other options include:
MEDIA CONTACT: Brian Kilen, Mayo Clinic Public Affairs, 507-284-5005, newsbureau@mayo.edu
- Antidepressant drugs ― These drugs are commonly used for multiple types of chronic pain, such as fibromyalgia, low back pain, headaches, diabetic neuropathy and other forms of nerve pain. In some people, antidepressants appear to help with pain, independent of their possible effect on depression. They can also improve depression symptoms, which can be caused by chronic, unrelieved pain. Antidepressants usually don’t lose their effect over time, and they may increase the effect of other pain drugs.
- Anti-seizure medications ― Several drugs developed primarily to control epileptic seizures have been found to help control stabbing or shooting pain that can result from nerve damage or impaired communication in the central nervous system. When a nerve is injured or functions abnormally, certain nerve receptors that communicate pain to the brain may fire inappropriately. Anti-seizure medications can help reduce this activity and decrease pain levels.
- Nonmedication strategies ― Using drugs to manage chronic pain usually works best as part of a larger plan that may include regular exercise, physical activity, physical therapy, counseling, stress management, massage and other components. Visiting a comprehensive pain rehabilitation center may be worth considering, especially for those who have struggled to find effective pain management. Reducing or eliminating unhelpful medications, often with a planned tapering of the drugs, is a common occurrence in pain rehabilitation programs.
Blood pressure guidelines refined for older adults, those with diabetes or kidney disease
Blood pressure guidelines have been refined for older adults and people with diabetes or kidney disease. The March issue of Mayo Clinic Health Letter covers these changes and why they were made.
High blood pressure is a common and serious health problem in the U.S. High blood pressure can lead to significant health risks including heart attack, stroke, heart failure and kidney failure and other organ damage. Older adults are particularly at risk. More than half of adults over age 65 and close to 80 percent of adults over age 75 have high blood pressure.
Normal blood pressure is considered to be less than 120/80 mm Hg. For some, high blood pressure tends to develop over many years without an exact cause. For others, an underlying condition, such as kidney or thyroid disease, causes high blood pressure.
The goal of treating high blood pressure is to keep it within a range that avoids damage to the arteries, heart, kidneys and brain. That range varies somewhat for subsets of patients.
The most recent guidelines, from the Eighth Joint National Committee on Prevention, Detection, Evaluation and Treatment of High Blood Pressure, were published in 2014. For those with high blood pressure, guidelines recommend blood pressure lower than:
- 150/90 mm Hg for healthy adults age 60 and older. This is slightly higher than previous guidelines.
- 140/90 mm Hg for healthy adults younger than 60.
- 140/90 mm Hg for adults with diabetes or kidney disease. This also is slightly higher than previous guidelines.
One of the underlying principles of the new guidelines is that more aggressive treatment isn’t always better at improving health, nor is it backed by solid evidence, especially in the case of older adults and those with diabetes or chronic kidney problems. Less aggressive treatment goals reduce the intensity of treatment, which also makes for fewer side effects.
It’s good to remember that guidelines are based on data derived from large numbers of carefully selected people ― and there are varying opinions on which blood pressure goals are best for optimal health. Patients should work with their providers to determine the best strategies to reduce the risk of heart disease, stroke and other consequences of high blood pressure.
Fostering thankfulness, improving well-being
Scientists are finding that people who are habitually grateful reap greater happiness, more positive relationships, increased sense of fulfillment and even sleep better, according to the March issue of Mayo Clinic Health Letter.
While everyone feels grateful at times ― for a gift, extra help, a rewarding job, or natural beauty ― transient moments of thankfulness aren’t enough to explain the wider concept of gratitude. Gratitude, especially as it correlates to a higher sense of well-being, focuses on noticing and appreciating the positive aspects of life. Practicing gratitude means being content in the moment, despite the imperfections of life.

Mayo Clinic doctor Amit Sood, M.D., has authored several books on training the brain to decrease stress, increase resilience and live meaningfully. Here are some of his suggestions to foster gratitude.
Start the day with gratitude: Begin the day by thinking of five people to whom you are grateful. The day starts on a more positive note when it begins with grateful thoughts.
Be thankful for simple things: Throughout the day, mentally note things easily taken for granted, electricity, running water, clean clothes or a cup of coffee.
Look for the positive in the negative: Try to see struggles as necessary forces that focus energy on what’s really important. Be thankful for a flexible mind that allows adversity to help you learn and grow.
Acknowledge your riches: If you are feeling bad, count your blessings, such as health, home, freedom, a job or loved ones.
Keep a gratitude journal: As you contemplate people and things you’re grateful for, write them down. Do it before you sleep so the last thoughts of the day are positive and sleep is restful. Refer back to the journal on rough days.
Say thank you: Express gratitude to others in words and deeds. Say thank you in person for a kind action or write a note to express gratefulness for having a person in your life.
###
Mayo Clinic Health Letter is an eight-page monthly newsletter of reliable, accurate and practical information on today’s health and medical news. To subscribe, please call 1-800-333-9037 (toll-free), extension 9771, or visit http://www.HealthLetter.MayoClinic.com
About Mayo Clinic Mayo Clinic is a nonprofit organization committed to medical research and education, and providing expert, whole-person care to everyone who needs healing. For more information, visit http://www.mayoclinic.org/about-mayo-clinic or https://newsnetwork.mayoclinic.org/.







