-
3 facts about acute lymphocytic leukemia in children

September is Childhood Cancer Awareness Month. The most common type of childhood cancer is acute lymphocytic leukemia (ALL), a blood and bone marrow cancer that creates immature white blood cells that can’t perform their typical functions. Because of this, the disease worsens quickly.
Most likely to occur in early childhood, ALL is more common in boys than girls, according to the American Cancer Society. Children younger than five are at highest risk for developing ALL.
Asmaa Ferdjallah, M.D., a Mayo Clinic pediatric hematologist and oncologist, treats children of all ages with ALL. Here’s what she wants families to know about this disease:
1. ALL is rare and has a collection of persistent symptoms.
In 2023, the American Cancer Society estimates that 6,540 new cases of ALL will be diagnosed in both children and adults. This represents less than half of 1% of all cancers in the U.S.
ALL symptoms vary and can resemble symptoms of flu and other common illnesses. Dr. Ferdjallah says most high fevers, swollen lymph nodes and bruises are part of typical childhood development. Parents should call their child’s healthcare professional if those symptoms persist, co-occur or seem unusual.
"With ALL, we often see frequent or daily high fevers that you can't explain," says Dr. Ferdjallah. "We'll often see rapid weight loss that doesn't make sense for a child's activity level. And we always ask about lumps or bumps, which can indicate swollen lymph nodes, as well as night sweats, bone pain and any new bruising or bleeding."
If your healthcare team suspects your child has ALL, they will draw blood for testing. "We would expect to see changes in blood counts" in a child with ALL, says Dr. Ferdjallah. "Low hemoglobin, low platelets, low neutrophils — having all these low blood counts may suggest ALL."
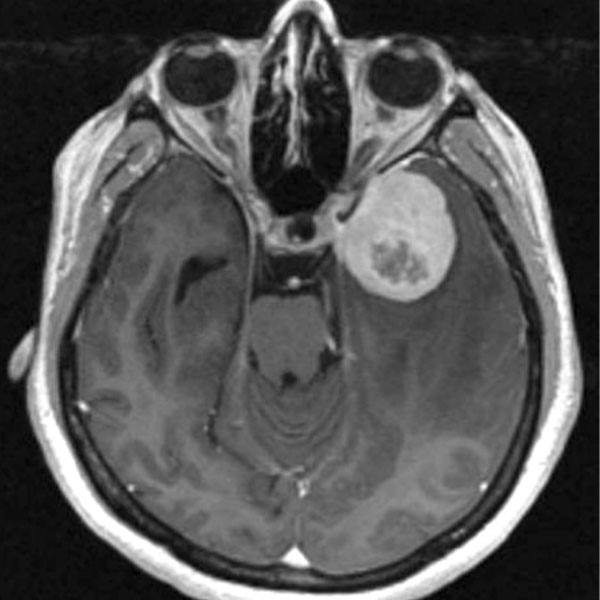
In addition to a blood test, healthcare professionals may also use a bone marrow test, imaging tests and a spinal fluid test to diagnose ALL.
Having one ALL symptom, such as a bruise or one low blood count, generally isn’t something to worry about, says Dr. Ferdjallah. "ALL declares itself. It’s not going to sneak up on you. It creates a constellation of symptoms that we see."
2. Children diagnosed with ALL have well-researched options for precision care.
Your child’s care team will consider many factors when determining the best treatment for ALL, including:
- The type of lymphocytes involved — B cells or T cells.
- The specific genetic changes present in the child’s leukemia cells.
- The child’s age.
- Lab test results, such as the number of white blood cells detected in a blood sample.
Care teams then tailor treatment plans for each patient based on factors that indicate standard risk or high risk for relapse. Called risk stratification, this approach to treatment has improved survival.
"Somebody with standard risk is usually between the ages of 1 and 10. A child in this age group with a white blood cell count of less than 50,000 is considered standard risk. Patients outside these parameters need more intense therapy and are considered high risk," says Dr. Ferdjallah.
For standard-risk patients, treatment typically involves chemotherapy given by infusion. "We also deliver chemotherapy into the spine via a spinal tap because we know some leukemias are very good at hiding in that space, and this can prevent relapses and later recurrences," says Dr. Ferdjallah.
Treatment can take two to three years, and the first few months are most intense.
"After the first six months, the patient enters a period called maintenance," says Dr. Ferdjallah. "Then we see patients less often because they need less intense therapy. Kids return to school, and their immune system is a little stronger. They can go on vacation, and their hair starts to grow back. ALL starts to feel like an annoying thing to manage and less like a life-altering, devastating illness."
The care team will perform a bone marrow biopsy to determine whether ALL is remission. "If there's no leukemia in the biopsy, that's the best sign that the patient is in remission, and that is associated with the best outcomes," says Dr. Ferdjallah.
There are many other options for children with high-risk genetic mutations or aggressive diseases for whom chemotherapy isn’t effective. ALL treatments may include targeted therapy, radiation therapy, bone marrow transplant, CAR-T cell therapy and clinical trials.
"We have multiple lines of therapy for these patients," says Dr. Ferdjallah. "Scientists and doctors have worked collaboratively for a long time to create networks, such as the Children’s Oncology Group, to conduct powerful clinical trials. The results of that research have informed us of the best therapy approaches," she says.
3. The outlook for kids diagnosed with ALL is excellent, and treatment options continue to improve.
The five-year survival rate for children with ALL is about 90%, and if a child remains cancer-free five years after treatment, they are likely cured.
"Children diagnosed with ALL do well in survivorship. They're able to live normal, healthy lives — get married, have kids, and have a normal life span," says Dr. Ferdjallah.
Meanwhile, available treatment options continue to improve.
"One of the most promising new treatment options is CAR-T cell therapy for pediatric patients, which uses a patient's T cells and genetically engineers them to target and kill their leukemia cells," says Dr. Ferdjallah. "That kind of therapy can save a patient from a stem cell transplant, which has more side effects and morbidity. We’ve seen good outcomes."
Dr. Ferdjallah is also excited about the development of new targeted therapies called monoclonal antibodies. "These drugs target mechanisms in leukemia cells that drive their ability to replicate quickly or damage normal tissues. (The drugs) tend to have fewer side effects than chemotherapy. That's exciting because it can improve quality of life," she says.
Dr. Ferdjallah wants families coping with a child’s ALL diagnosis to know there is good reason to hope. "It’s completely horrifying to think about your child having cancer, but the No. 1 thing I want parents to hear is that ALL is one of the most curable cancers. And we've come a long, long way with therapies."
Learn more
Learn more about ALL and find clinical trials at Mayo Clinic.
Join the Blood Cancers and Disorders Support Group or the Caregivers Support Group on Mayo Clinic Connect, an online community moderated by Mayo Clinic for patients and caregivers.
This article first published on the Mayo Clinic Comprehensive Cancer Center blog.