-
Global study finds metabolic syndrome increased risk of acute respiratory distress syndrome, death in patients hospitalized with COVID-19
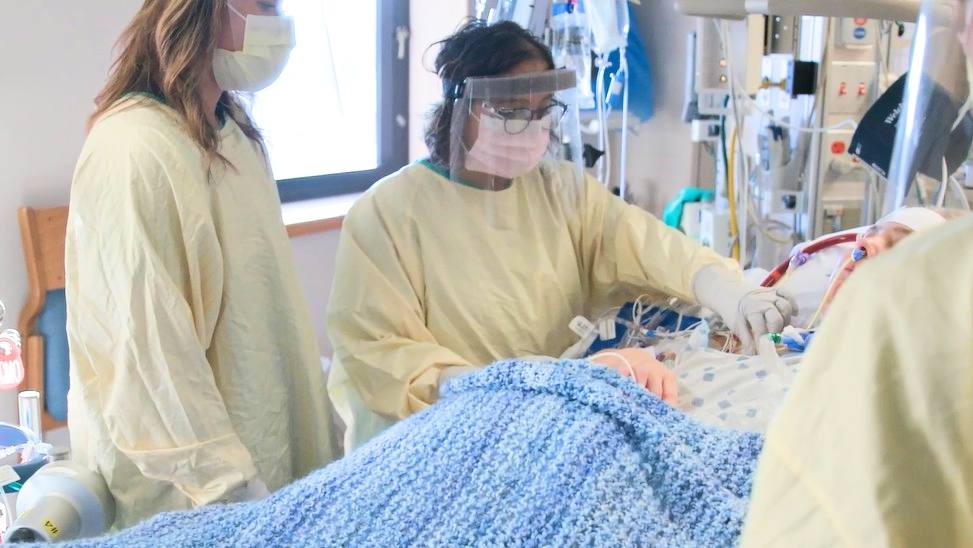
ROCHESTER, Minn. ― Patients hospitalized with COVID-19 who had a combination of high blood pressure, obesity, diabetes, or other conditions associated with metabolic syndrome were at much higher risk of acute respiratory distress syndrome and death, according to an international study published in JAMA Network Open.
The risk for developing acute respiratory distress syndrome, a life-threatening lung condition that causes low blood oxygen, grew progressively higher with each additional metabolic syndrome criteria present. The study, one of the largest to examine the link between metabolic syndrome and outcomes for COVID-19, examined records of more than 46,000 patients admitted in 181 hospitals across 26 countries.
“Our study found that if you have high cholesterol, high blood pressure, mild obesity and pre-diabetes or diabetes and are hospitalized with COVID-19, you have a one in four chance of developing ARDS, which is significant,” said lead author of the study Dr. Joshua Denson, pulmonary and critical care medicine physician and assistant professor of medicine at Tulane University School of Medicine. “We also found that at every level of respiratory support, patients with metabolic syndrome experienced worse outcomes. Metabolic syndrome patients experienced increased invasive mechanical ventilation, increased noninvasive ventilation, or high-flow oxygen support, and increased supplemental oxygen use compared to patients without metabolic syndrome.”
Researchers from Mayo Clinic, the Society of Critical Care Medicine, and Tulane University followed outcomes for patients hospitalized between mid-February 2020 to mid-February 2021 in the Discovery VIRUS: COVID-19 Registry. Researchers compared 5,069 patients (17.5%) with metabolic syndrome with 23,971 control patients (82.5%) without metabolic syndrome. They defined metabolic syndrome as having more than three of these criteria: obesity, prediabetes or diabetes, hypertension, or high cholesterol.
Patients with metabolic syndrome were 36% more likely to develop acute respiratory distress syndrome, almost 20% more likely to die in the hospital, more than 30% more likely to be admitted to an ICU, and 45% more likely to require mechanical ventilation. Researchers calculated these risks after adjusting for race, age, sex, ethnicity, other comorbidities and hospital case volume.
Overall, slightly more than 20% of the patients with metabolic syndrome died in the hospital, 20% developed acute respiratory distress syndrome and almost half were admitted to the ICU. Approximately 16% of those without metabolic syndrome died, 12% developed acute respiratory distress syndrome, and nearly 36% were admitted to the ICU.
Metabolic syndrome was significantly more common among patients with COVID-19 admitted to U.S. hospitals (18.8%) than those admitted to non-U.S. hospitals (8%). According to the Centers for Disease Control and Prevention, more than one-third of adults in the U.S. meet the criteria for metabolic syndrome, with some regions having a metabolic syndrome prevalence greater than 40%.
Severe cases of COVID-19 are characterized by a hyperinflammatory immune response to the infection throughout the body. Authors suspect that chronic low-grade inflammation from metabolic diseases, mainly when clustered together, could make these patients more vulnerable to COVID-19.
The researchers note that given the high rates of metabolic syndrome, obesity and diabetes in the U.S., one hypothesis for why the U.S. leads the world in COVID-19 cases and deaths could be the high prevalence of metabolic syndrome in this population.
"These important findings are another example of possibilities from pooled data of hundreds of hospitals in detecting meaningful associations during the pandemic," says Rahul Kashyap, M.B.B.S., senior author of the study and principal investigator of the Discovery VIRUS: COVID-19 Registry. "These findings will assist with efforts for creating national infrastructures for identifying critical illness risk factors and testing novel/repurposed medications to help improve patient outcomes." VIRUS stands for Viral Infection and Respiratory Illness Universal Study.
This study was made possible by the Viral Infection and Respiratory Illness Universal Study. This study reveals practice variations and provides a rich database for research into effective treatments and care. In March 2020, the Society of Critical Care Medicine and Mayo Clinic launched this first global COVID-19 registry that tracks ICU and hospital care patterns in near real time. For more information, visit the Discovery VIRUS: COVID-19 Registry.
###
About Mayo Clinic
Mayo Clinic is a nonprofit organization committed to innovation in clinical practice, education and research, and providing compassion, expertise and answers to everyone who needs healing. Visit the Mayo Clinic News Network for additional Mayo Clinic news. For information on COVID-19, including Mayo Clinic's Coronavirus Map tracking tool, which has 14-day forecasting on COVID-19 trends, visit the Mayo Clinic COVID-19 Resource Center.
About the Society of Critical Care Medicine
The Society of Critical Care Medicine (SCCM) is the largest nonprofit medical organization dedicated to promoting excellence and consistency in the practice of critical care. With members in more than 100 countries, SCCM is the only organization that represents all professional components of the critical care team. SCCM’s Discovery network fosters collaborative research to improve outcomes for critically ill and injured patients and seeks to incorporate findings into practice using SCCM's broad base of programs. Visit sccm.org for more information. Follow @SCCM or visit us on Facebook.
About Tulane University School of Medicine
One of the nation's most recognized centers for medical education, Tulane University School of Medicine is a vibrant center for education, research and public service. As the second-oldest medical school in the Deep South and the 15th oldest medical school in the United States, it recruits top faculty, researchers and students from around the world. Tulane pushes the boundaries of medicine with groundbreaking life science and clinical advances and is dedicated to equipping the next generation of medical professionals with the tools to succeed in the rapidly changing future of health care.
Media contacts:
- Colette Gallagher, Mayo Clinic Public Affairs, newsbureau@mayo.edu
- Keith Brannon, Director, Tulane University Public Relations, kbrannon@tulane.edu
- Melissa Nielsen, Senior Marketing and Communications Manager, The Society of Critical Care Medicine, mnielsen@sccm.org
Related Articles