-
Mayo Clinic expert speaks of significance of Lyme disease uptick
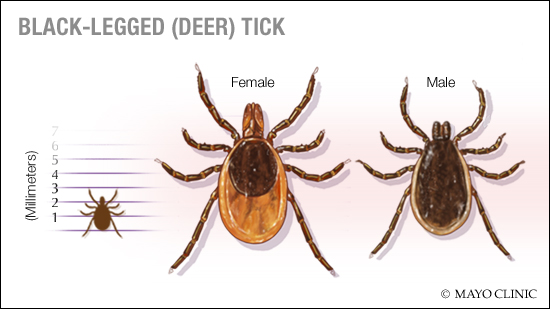
Lyme disease has infected more than 14% of the world's population, according to a new study. "It's significant," says Dr. Bobbi Pritt, director of the Clinical Parasitology Laboratory at Mayo Clinic.
"If you look at the numbers and how it breaks down in regions across the United States, in some areas, that exceeds 50% seropositivity. That means people are walking around with antibodies in their blood that are detectable. That shows they've been exposed to Lyme disease at some point in their life," says Dr. Pritt. "Now whether it was in the past and they've been successfully treated, or whether they have it right now, you can't tell by that result, but it's a marker of exposure."
Watch: Dr. Bobbi Pritt talks about Lyme disease.
Journalists: Broadcast-quality soundbites are available in the downloads at the bottom of the post. Please courtesy: "Mayo Clinic News Network."
"It's very helpful for people to know that Lyme disease is not just a problem we have in the United States. And that it, of course, goes up into Canada, but also that in Europe and Asia, they also have Lyme disease," says Dr. Pritt.
"And as we raise awareness, there will hopefully be more studies like this to look at where people are getting exposed to Lyme disease, and how many people have been infected in the past. We need to understand the disease and where it is so that we can work on better ways to detect and treat it," she says.
Lyme disease
Lyme disease is a bacterial infection spread by an infected tick. Patients may present with a rash at the site of the tick bite — classically with a bull's-eye rash. But that's not always the case.
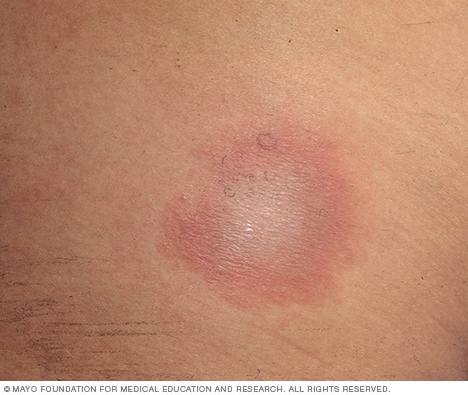
"Also, some people may have a rash and not know if it's on the back of their head or another hard-to-see and hard-to-reach area. If the infection is not treated right away, the patient may then progress to having other symptoms like disseminated rashes, joint pain, arthritis and even neurologic involvement. And they can even have one-sided facial paralysis called Bell's palsy."
Lab tests help confirm or rule out diagnoses of Lyme disease. Mayo Clinic Laboratories perform more than 300,000 tests for tick-borne diseases each year, says Dr. Pritt.
When to seek medical care
Finding a tick on you and removing it promptly is not a reason to seek medical attention, especially for those who live in an area where ticks are a daily occurrence, says Dr. Pritt.
"If a patient lives in an area where there's a lot of Lyme disease, finding a tick that's been attached to them for more than 24 hours, ideally more than 36 hours, that in and of itself is enough to prompt them to go to their physician to see if they should get some antibiotics to prevent Lyme disease," she says.
Dr. Pritt says "If someone were to present with any type of illness during the spring, summer or fall months when they been exposed to ticks, where they may have a
rash, a headache, a fever, those could all be signs of tick-borne diseases, Lyme disease and other diseases. And that should prompt them to go to their physician."
Prevention
The best way to avoid Lyme disease is to avoid getting a tick bite. Dr. Pritt says it's important for people to protect themselves from tick bites. Avoiding tick bites will protect them not just from Lyme disease, but also many other tick-borne infections.
Note these tick prevention tips:
- When possible, avoid areas where ticks are frequently found.
- Use a repellent with 30% or more of DEET.
- Wear clothing that covers your arms and legs.
- Tuck pants into socks while hiking.
"I also like oil of lemon eucalyptus, which has been shown by the Environmental Protection Agency to be almost as effective as DEET and smells a little better. Also, wearing permethrin sprayed on clothing is helpful. That also will repel and even kill ticks. And then just covering up with clothing so that the ticks can't get to your skin. If you tuck your pants into your socks, you're taking away an avenue for ticks to get to your legs to bite you."
Related posts:
- "Mayo Clinic Minute: How to avoid ticks."
- "Tick-borne infections and the complicated role of climate change."
- "Rare Lyme disease-causing bacteria spotted on routine blood films."
For the safety of its patients, staff and visitors, Mayo Clinic has strict masking policies in place. Anyone shown without a mask was recorded prior to COVID-19 or recorded in an area not designated for patient care, where social distancing and other safety protocols were followed.







