-
Mayo Clinic Q and A: Cellulitis can be life-threatening, so prompt treatment is key
 DEAR MAYO CLINIC: What causes cellulitis, and how is it treated?
DEAR MAYO CLINIC: What causes cellulitis, and how is it treated?
ANSWER: Cellulitis is a bacterial infection that typically affects the deeper layers of your skin and the layer of fat just beneath. It’s quite common, especially among middle-aged and older adults. Most often, cellulitis occurs when a crack or cut in your skin allows bacteria to get inside and multiply.
Cellulitis can range from mild to severe. Most cases are treated effectively with antibiotics. Prompt treatment is key. If severe, or when left untreated, cellulitis can spread to your lymph nodes, bloodstream and deeper tissues, rapidly becoming life-threatening.
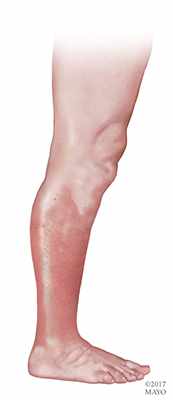
Cellulitis usually develops in the lower legs, although it can occur in any area with skin. The surface skin area appears red and swollen, and is typically painful and warm to the touch. Over time, the untreated area of redness expands.
Certain factors can put you at greater risk of cellulitis, including:
- Wounds, cuts or incisions
Any opening in the skin — from a small scratch or an insect bite to an ulcer or a recent surgery — can provide an entryway for bacteria.
- Skin condition
Conditions such as athlete’s foot, dermatitis and eczema can cause the skin to break or crack, and increase your chance of developing cellulitis. Shingles can cause broken blisters that are vulnerable to infection. Itching leads to scratching, and scratching introduces bacteria to deeper layers.
- Swelling
Skin can become swollen because of damage to your veins (edema) or the lymphatic system (lymphedema) or following surgery. Stretched, swollen skin can crack, creating an entry point for bacteria.
- Previous episodes
Having had cellulitis in the past increases your chances of having it again.
- Peripheral neuropathy
Decreased sensation and an inability to feel an injury can increase the risk of cellulitis.
- Other illnesses
Certain conditions such as diabetes or cancer can make you more prone to infection because of poor circulation or a weakened immune system. With diabetes, keeping blood sugars in control can reduce the risk of nerve or blood vessel diseases, as well as severity of cellulitis.
If you develop signs or symptoms of cellulitis, see your doctor as soon as possible. If symptoms are worsening or you also have a fever or chills, seek emergency care, because the infection may be severe or spreading rapidly.
To make a diagnosis, your health care provider likely will review your medical history and perform an exam to look for skin features that suggest cellulitis. If signs such as redness and swelling are developing on both legs, the cause is usually something other than cellulitis. Sometimes blood tests or imaging are necessary to rule out other conditions, including a blood clot in a leg vein (deep-vein thrombosis), a reaction to a drug or a skin irritant, lymphedema, or an infected joint. For simple, uncomplicated cellulitis, however, additional testing isn’t required.
Cellulitis usually improves with antibiotic treatment in combination with local cares (elevation and compression) that reduce swelling. Decreased swelling improves blood supply and circulation, getting the antibiotic to the infection and making the antibiotic more effective. Also, cool compresses can relieve discomfort.
Typically, antibiotics are taken for five to 14 days, depending on the severity and location of the infection and response to treatment. Most people start to feel better within two or three days of starting treatment; however, it is recommended that patients complete the entire course of antibiotic prescribed to ensure the infection resolves and the bacteria are eliminated.
Treating underlying conditions that make you more vulnerable to cellulitis, such as edema, eczema and diabetes, is also helpful in clearing up the present infection and preventing a recurrence.
More serious infections may require hospitalization for administration of antibiotics via IV and close monitoring for complications and improvement. While complications are rare, they can be serious and life-threatening. Sometimes, severe cellulitis can cause the surrounding tissue to die. Rarely, bacteria can enter the bloodstream, spreading the infection to distant parts of the body.
If you have recurring episodes of cellulitis, your doctor may recommend taking a long-term course of preventive antibiotics to keep the infection at bay. It also may help to visit with a dermatologist or an infectious disease specialist to look for other causes of your symptoms. (adapted from Mayo Clinic Health Letter) — Dr. Marcia O’Brien, Family Medicine, Mayo Clinic, Rochester, Minnesota