-
Featured News
Mayo Clinic Q and A: Diagnosing Parkinson’s disease
 DEAR MAYO CLINIC: My mother was recently diagnosed with Parkinson’s, but she doesn’t have many symptoms. I would like her to get a second opinion. Is there a blood test that can determine if the diagnosis is accurate?
DEAR MAYO CLINIC: My mother was recently diagnosed with Parkinson’s, but she doesn’t have many symptoms. I would like her to get a second opinion. Is there a blood test that can determine if the diagnosis is accurate?
ANSWER: There’s no one test that can be used to diagnose Parkinson’s disease. Instead, the diagnosis is based on a person’s medical history and symptoms, along with a neurological and physical exam. If your mother has doubts about her Parkinson’s diagnosis, getting a second opinion from a neurologist who specializes in the disease would be reasonable.
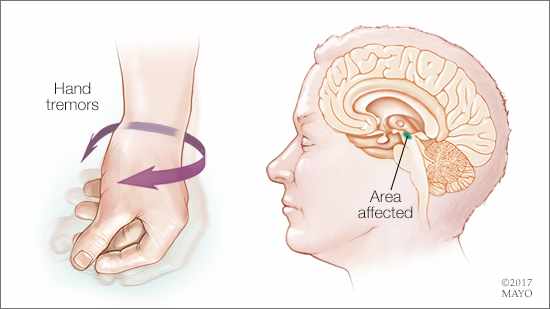
Parkinson’s disease is a progressive disorder of the nervous system that affects movement. In people who have this disease, certain nerve cells in the brain, called neurons, gradually die.
Many Parkinson’s symptoms are related to the loss of brain neurons that produce a chemical messenger called dopamine. Loss of dopamine can lead to a variety of symptoms. Those symptoms can vary widely from person to person. Parkinson’s develops slowly over time. In the disease’s early stages, symptoms may be very mild and barely noticeable.
About 80 percent of people with Parkinson’s have some type of tremor, or shaking, in a limb. It typically first affects a hand or fingers. Over time, Parkinson’s often makes it difficult to move quickly and causes muscle stiffness, limiting a person’s range of motion and sometimes causing pain. This can lead to a shuffling gait with short steps. It slows basic daily tasks, such as rising from a chair, writing or dressing. Some people with Parkinson’s develop a stooped posture and feel unsteady.
Parkinson’s typically impairs a person’s normal spontaneous body movements, such as blinking, smiling or swinging the arms while walking. The loss of dopamine that happens in Parkinson’s may sometimes trigger sleep disorders, panic attacks, anxiety or insomnia.
Neurologists review these symptoms when considering a diagnosis of Parkinson’s disease. Brain imaging or blood tests may be recommended, but, often, the diagnosis is made based on the features identified at an office visit. When a health care provider strongly suspects Parkinson’s after an initial evaluation, he or she may prescribe carbidopa-levodopa. This drug helps replace dopamine in the brain.
If symptoms substantially improve when a person takes carbidopa-levodopa, that’s usually a clear sign that Parkinson’s is causing those symptoms. The changes don’t happen within a day or two, though. To be most effective, a person must take the medication in the correct dose over a longer period of time.
Among people with fully developed Parkinson’s disease, an accurate diagnosis that leads to appropriate carbidopa-levodopa dosage is crucial. For most patients, treatment also involves an exercise program to increase fitness and improve muscle strength, flexibility and balance.
Although there is no cure for Parkinson’s disease, in most cases, the disease and its symptoms can be managed effectively, so those who have Parkinson’s are able to continue engaging in active, fulfilling lives. — Dr. J. Eric Ahlskog, Neurology, Mayo Clinic, Rochester, Minnesota