-
Cancer
Mayo Clinic Q and A: Lung cancer — symptoms and prevention
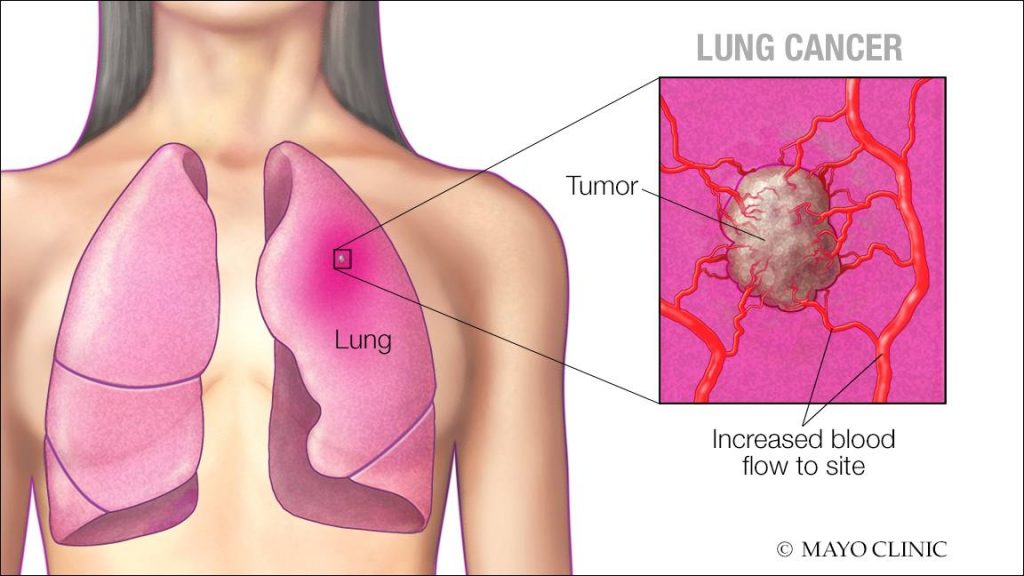 DEAR MAYO CLINIC: Are there ever any early signs of lung cancer, or is it usually found only in the later stages? Can anything be done to prevent it other than not smoking?
DEAR MAYO CLINIC: Are there ever any early signs of lung cancer, or is it usually found only in the later stages? Can anything be done to prevent it other than not smoking?
ANSWER: It’s rare for lung cancer to trigger symptoms before it progresses to its later stages. Most cases of early-stage lung cancer are detected by chance in people without symptoms who have a chest imaging study for other reasons. Not smoking or quitting smoking still is the most effective way to prevent lung cancer. But there are other steps you can take that contribute to long-term lung health.
Lung cancer remains the leading cause of cancer deaths in the U.S., among both men and women. Typical symptoms, which usually appear only when the disease is advanced, include a persistent cough, shortness of breath, chest pain, coughing up blood and hoarseness.
Smoking is by far the most common cause of lung cancer. People who smoke make up about 85 percent of lung cancer cases. Lung cancer risk for smokers goes up with the amount a person smokes each day, along with the number of years of smoking.
Nonsmokers who may be at an increased risk for developing lung cancer include individuals who have prolonged exposure to secondhand smoke, long-term exposure to radon gas, workplace exposure to asbestos and other substances known to cause cancer, and people who have a family history of lung cancer.
The best way to avoid lung cancer is not to smoke. Quitting at any age significantly lowers the risk of developing lung cancer. Longtime current smokers and prior smokers also may benefit from newly established lung cancer screening programs.
Screening is used to detect lung cancer in people at high risk for the disease before symptoms appear. It involves an imaging test — known as a low radiation dose CT scan of the lungs — to look for signs of cancer, specifically pulmonary nodules. If cancer is found at an early stage, it’s more likely to be able to be successfully treated. Lung cancer screening has been shown to save lives, similar to breast cancer and colon cancer screening using mammography and colonoscopy, respectively.
In general, screening is recommended for people 55 to 80 who have smoked for 30 pack years or more. Pack years are calculated by multiplying the number of packs of cigarettes smoked a day and the number of years smoked. Screening may be appropriate for other individuals at increased risk for lung cancer, too. If you think you may fall into one of those categories based on your health history, family history or exposure to cancer-causing substances, talk to your health care provider about screening. A national study conducted in 2011 found that annual lung cancer screening for high-risk individuals significantly reduced lung cancer-related deaths in that population.
Beyond not smoking, taking steps to reduce your exposure to radon also may lower your lung cancer risk. Radon is created by the natural breakdown of uranium in soil, rock and water. If you live in an area where radon is common, have your home tested for it. For information on radon testing, contact your local department of public health or a local chapter of the American Lung Association.
If your work involves exposure to toxic substances, take steps to protect yourself. Follow your employer’s precautions. For example, if you’re given a face mask for protection, always wear it.
Finally, a healthy, active lifestyle that includes regular exercise and a diet rich in fruits and vegetables can boost your immune system and lower your risk for many types of cancer, including lung cancer.
If you’re concerned about developing lung cancer, talk to your health care provider. He or she can evaluate your overall risk and help determine if there are steps you can take to lower that risk. — Dr. Tobias Peikert, Pulmonary and Critical Care Medicine, Mayo Clinic, Rochester, Minnesota







