-
Featured News
Mayo Clinic Q and A: Models using 3-D printing often a valuable tool for surgeons
 DEAR MAYO CLINIC: I’ve heard that doctors can now use 3-D printing to prepare for some kinds of surgery. How does that work? When is it used?
DEAR MAYO CLINIC: I’ve heard that doctors can now use 3-D printing to prepare for some kinds of surgery. How does that work? When is it used?
ANSWER: Using 3-D-printed models to prepare and plan for surgery is becoming more common. These life-size, patient-specific models can be valuable tools for surgeons as they decide what approach and techniques will be best for a specific surgery. The models are particularly helpful for procedures that may be new, uncommon or complex. These 3-D models also play an important role in education.
The models are created with a printing press that takes information from a patient’s imaging scans, such as a CT or an MRI. Then, layer by layer, this printing press produces a 3-D model of the patient’s anatomy. Typically, the models are made from a type of polymer or plastic. In some cases, 3-D models are fashioned out of soft material, so surgeons can practice the surgical technique on the model first — an approach that can increase accuracy during the procedure.
Because 3-D models are life-size, they recreate a patient’s individual anatomy. Therefore, surgeons can hold and rotate the models in their hands to get a better sense of how they need to position a patient on the table during the operation, and determine where they should make surgical incisions. Surgeons also can determine whether there may be different surgical approaches they hadn’t thought of or didn’t think were possible when they were studying the case on traditional two-dimensional imaging. Examining 3-D models frequently reveals quirks of a patient’s anatomy that change the course of the surgery.
The technology often is used for surgeries that involve the head and neck. It can be especially helpful when planning complex facial or airway reconstruction. The 3-D models also are becoming more common for a range of other surgeries, including heart and lung surgery, joint reconstruction, and tumor resections.
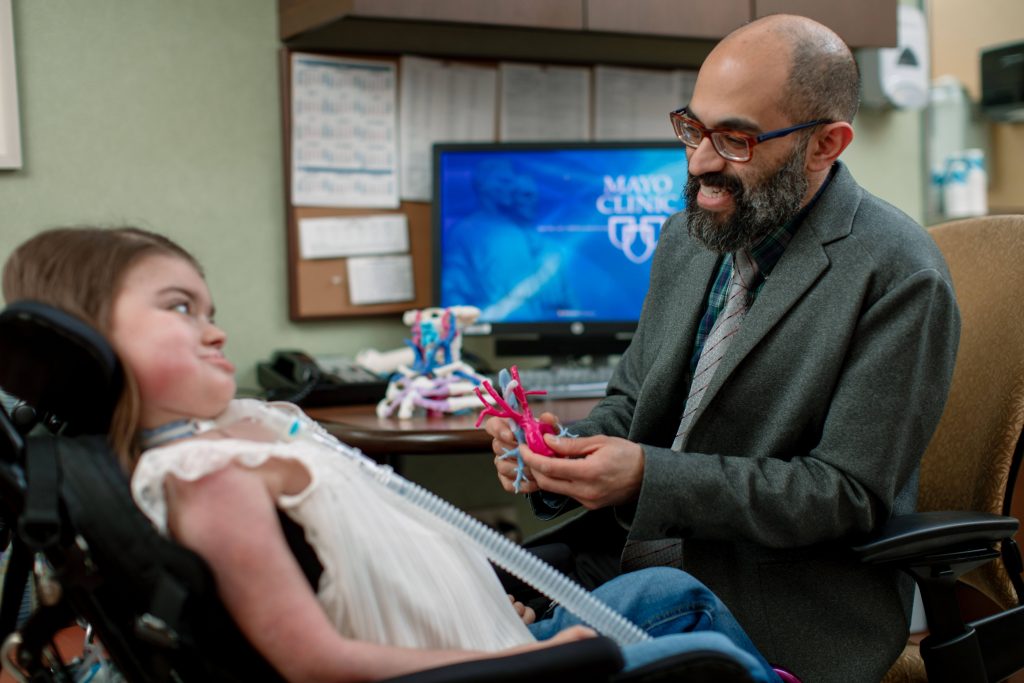
In addition, 3-D models take away some of the unknowns that otherwise could be part of a surgical procedure, and having these models facilitates communication among the surgical team. The 3-D models also can serve as teaching tools for surgical trainees. And they aid in patient education, too. Before patients undergo surgery, they can view their 3-D models. Seeing an anatomically correct model of their inner structures gives patients a better sense of what’s going to happen during surgery.
There are some drawbacks to using these models. The printing process is slow, and it can be expensive. A small model may take four to six hours to create, while a large, complex model might take up to 24 hours. Using the models requires additional time for planning and preparation before a surgical procedure. Not all health care organizations have the resources needed to offer 3-D printing and models, though the technology is becoming less expensive and more accessible over time. But, overall, the potential that 3-D models have for improving surgical outcomes is vast and far outweighs the drawbacks.
Eventually, it may be possible to routinely use this technology not only to produce models of a patient’s anatomy, but also to make custom-designed structures to be implanted into patients during surgery. For example, a 3-D printer could produce a stent that would fit precisely into a patient’s heart, or a tailored endotracheal tube could be created for a patient who needs long-term breathing assistance. A few cases of 3-D-printed airway stents have been reported. In some cases, 3-D technology already is aiding in the creation of artificial joints and other implants customized to individual patients. In short, the future of 3-D printing for surgery looks promising indeed. — Dr. Karthik Balakrishnan, Pediatric Otorhinolaryngology, Mayo Clinic, Rochester, Minnesota