-
Featured News
Mayo Clinic Q and A: Sex after menopause

DEAR MAYO CLINIC: I went through menopause a few years ago and didn’t have any of the usual signs or symptoms. But, lately, I'm finding that my vaginal area is extremely dry, and sex is becoming uncomfortable ─ even with a lubricant. Are there other options?
ANSWER: Your situation is common. Menopause can trigger a wide variety of symptoms, but not everyone has all of them, and different symptoms of menopause tend to develop at different times. Vaginal dryness often doesn’t appear until a year or two after the last menstrual cycle. You have several options, in addition to a lubricant, that can ease your discomfort.
When you go through menopause, your body experiences a significant drop in the amount of the hormone estrogen it makes. The loss of estrogen can lead to a number of symptoms that affect the urinary tract and genital area.
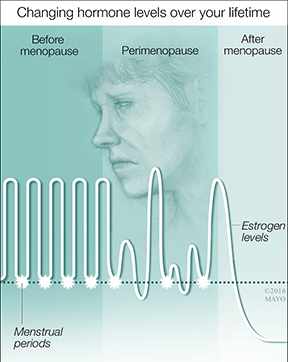
Those symptoms may include burning with urination, an increase in urinary frequency, an urgent need to urinate, incontinence associated with urgency, increased risk for urinary tract infections, and vaginal dryness, itching or burning. In addition to being drier after menopause, vaginal tissues often become thinner and less elastic. Because of these changes, sex may not only be uncomfortable, it may be painful. Together, all of these symptoms are known as genitourinary syndrome of menopause, or GSM.
According to the North American Menopause Society, up to 45 percent of women have symptoms of GSM after menopause, including painful sex due to vaginal dryness. Less than a quarter of those women go to their medical providers to try to do something about it. But, help is available.
You mention that you use a vaginal lubricant. That over-the-counter product is designed to be applied before sexual activity to make sex more comfortable and pleasurable. When a lubricant is not enough, consider using a vaginal moisturizer, too. This product is also available without a prescription at most drug stores and pharmacies. You apply it once every two or three days to maintain vaginal moisture.
If you use a moisturizer and a lubricant, but sex is still uncomfortable or painful, make an appointment to talk to your medical provider about prescription therapies for vaginal dryness. He or she may recommend treatment with low-dose vaginal estrogen. It comes in several forms, including a cream you apply twice a week, tablets placed into the vagina twice a week, and a ring that’s inserted in the vagina and replaced every three months.
Another option is an oral medication called ospemifene. It’s a selective estrogen receptor modulator, or SERM, that’s approved for treating painful intercourse associated with GSM. While this medication is an option for most women, it isn’t recommended for women who have breast cancer or are at high risk of developing breast cancer. Your medical provider can help you find a treatment for vaginal dryness based on your symptoms and personal preferences, as well as your medical and family history.
Your medical provider also can talk with you about any other menopause symptoms you may have and discuss ways to ease those, as well. Hormone therapy, which remains the most effective treatment for hot flashes and night sweats related to menopause, is appropriate for many women. Its use depends on your age, how long it’s been since menopause began, and your personal health history, among other factors. In a conversation with your medical provider, you can sort through what’s best for you. — Dr. Stephanie Faubion, Women’s Health Clinic, Mayo Clinic, Rochester, Minnesota