-
Featured News
Mayo Clinic Q and A: Stem cell therapy for arthritis
 DEAR MAYO CLINIC: What’s the latest information on using stem cell therapy to treat an arthritic shoulder that causes excessive pain?
DEAR MAYO CLINIC: What’s the latest information on using stem cell therapy to treat an arthritic shoulder that causes excessive pain?
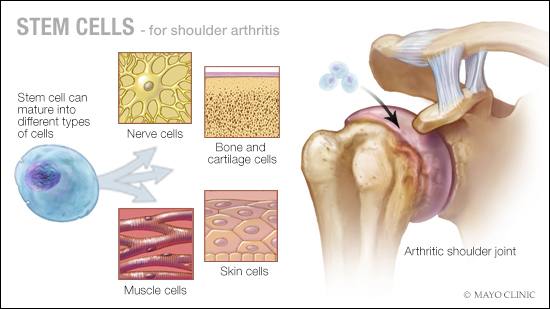
ANSWER: New efforts in regenerative medicine, including stem cell therapy, could dramatically affect orthopedic surgery over the coming years. Much of this hope is pinned on using stem cells to treat degenerative conditions such as shoulder arthritis. Although it shows promise, stem cell treatment for arthritis isn’t widely available at this time, as it’s still being researched.
Stem cells are the basic building blocks of all human tissue. Stem cells hold potential as treatment, in part, because they can communicate valuable information about tissue growth and healing to other cells in the body. Arthritis involves joint degeneration due to loss of the cartilage that cushions bones. Recently researchers have begun to look to stem cells for orthopedic conditions such as shoulder arthritis. Progress using stem cells to treat arthritis already has been reported, with the ultimate goal of using stem cells to regrow cartilage.
When discussing stem cell therapy, it’s important to understand that pure stem cells are not currently available to U.S. patients outside of a clinical research study. A handful of clinical research trials, monitored by the U.S. Food and Drug Administration (FDA), are ongoing at this time to study stem cell treatment for arthritis. The early findings from these trials are encouraging.
Unfortunately, the excitement surrounding emerging stem cell therapy has led some patients and health care providers to overlook the lack of scientific evidence to support its use at this time. Stem cell therapies currently used outside clinical studies do not contain pure stem cells. Instead, they are a mix of a variety of cells, of which only a very small percentage are stem cells. It is possible that many of these treatments do not contain enough stem cells to help.
It is also important to recognize that many stem cell therapies now marketed directly to patients are conducted without the required biologics license from the FDA. Also, some forms of mislabeled stem cell therapies do not contain any living stem cells. Such practices are cause for concern, as these treatments can mislead patients and the public, and delay the scientific progress needed to turn stem cell therapies into cures.
What the research into stem cells and arthritis shows is that there are opportunities for stem cell treatment to be used as injection therapy alone and in addition to orthopedic surgical procedures. Successful stem cell therapies thus far have resulted mostly in pain relief and improvement in function or quality of life. Only a few limited early studies have demonstrated improvement in new cartilage or bone formation needed to cure arthritis. Exactly how that cartilage regrowth occurs, or even how pain relief is achieved, is still unknown. That means if you have a stem cell procedure, it will be used to treat the symptoms of arthritis only. The ability to cure the disease entirely is not yet available.
No major research studies have specifically investigated stem cell treatment for shoulder arthritis. Much of what is known about stem cells in arthritis comes from research into knee degeneration. It’s not known if the successes treating knee arthritis will prove to be similarly beneficial when used for the shoulder. Therefore, current recommendations to treat shoulder arthritis remain the judicious use of gentle pain relievers, exercise and occasional steroid injections. In severe cases, shoulder replacement can provide long-lasting pain relief.
With demonstrable safety and mounting evidence of the effectiveness of stem cell therapy for some orthopedic conditions, potentially all orthopedic disease could be treated with stem cell therapy in the future. But, first, doctors and patients will have to wait until the scientific evidence catches up to the excitement around this promising option. — Dr. Shane Shapiro, Orthopedic Surgery and Center for Regenerative Medicine, Mayo Clinic, Jacksonville, Florida