-
Health & Wellness
Mayo Clinic Q and A: Understanding chronic kidney disease
DEAR MAYO CLINIC: I was diagnosed with chronic kidney disease but did not have any symptoms, so far as I knew. Are there early symptoms that I missed? Is this hereditary? Should I be advising family members? Is this curable? Am I at risk for other issues?
ANSWER: In its early stages, chronic kidney disease rarely causes noticeable symptoms. Kidney disease happens when the kidneys have been damaged and no longer work as they should.
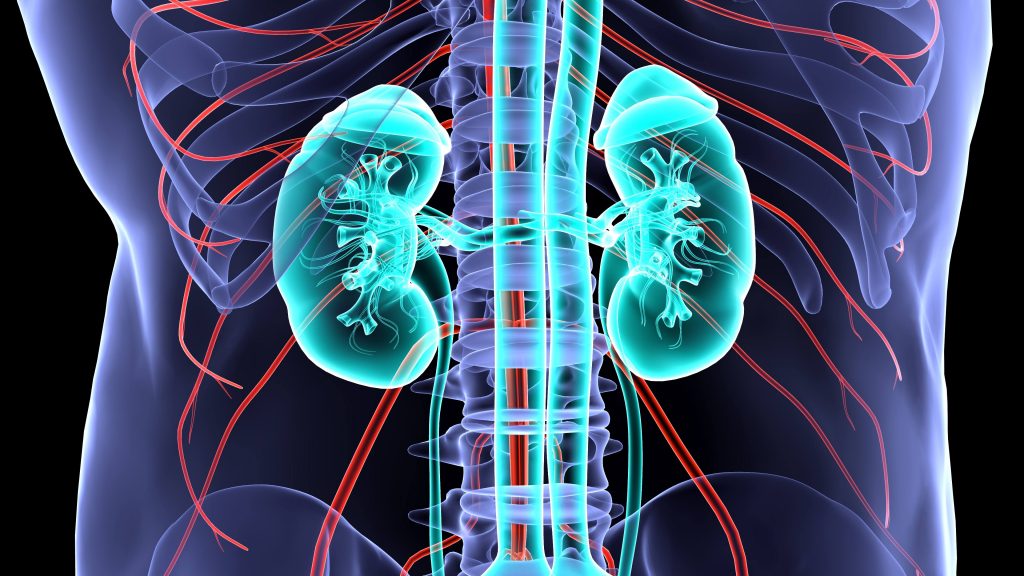
Kidneys are two bean-shaped organs, each about the size of a fist, located in the back of your abdomen on either side of your spine. The main job of the kidneys is filtering waste and excess fluid from the blood into what becomes urine. Kidneys also perform other tasks, such as adjusting the balance of minerals and acids in the blood, regulating blood pressure, and sending signals to bone to make red blood cells.
Although genetics may play a role in its development, chronic kidney disease is most commonly the result of either diabetes or high blood pressure. When diagnosed early, there are often steps that can minimize the damage and slow the progress of chronic kidney disease.
As in your situation, it's common for kidney disease not to cause any noticeable symptoms when it first develops. As the disease worsens, symptoms may appear, although they often are vague and may be overlooked.
Symptoms may differ depending on the cause of kidney damage or how advanced the damage may be. Symptoms can include fatigue; shortness of breath; poor appetite; nausea; and swelling of the hands, legs and ankles.
Persistently foamy urine can be a telltale sign of damage of the filtering apparatus in your kidneys. As your kidneys filter blood, they take out waste products, while keeping substances your body needs, such as proteins. When your kidneys are damaged, they may not be able to retain proteins properly, and high levels of protein pass into your urine. The extra protein causes urine to become foamy. This typically happens in kidney disease states such as glomerulonephritis (inflammation of the tiny filters in your kidneys), vasculitis (inflammation of the blood vessels in the body) or advanced diabetic kidney disease.
Chronic kidney disease tends to run in families, so some people are genetically more likely to develop the disease. Genetic disorders, such as autosomal dominant polycystic kidney disease, can lead to kidney failure in multiple family members. Chronic kidney disease is more common in certain groups, including African Americans, Native Hawaiians, Pacific Islanders, Native Americans and Asian Americans. People with mutations in the apolipoprotein L1 (APOL1) gene have a higher chance of kidney disease, and these mutations have been found in persons with ancestors from Africa.
A more significant risk factor for chronic kidney disease than genetics alone, however, is having a medical condition that could harm your kidneys. The two most common conditions are high blood pressure and diabetes. If left untreated, over time, these diseases can weaken the tiny blood vessels within the kidneys that filter waste from the blood, making them unable to work properly. It is important, if you have been diagnosed with diabetes or high blood pressure, that you work with your health care team to ensure these conditions are under good control.
Other conditions that can lead to chronic kidney disease include polycystic kidney disease, recurrent kidney infections, obstruction of the urinary tract, and disorders that cause inflammation within the kidneys, such as glomerulonephritis and interstitial nephritis. Some medications can affect kidney function, too. Finally, chronic kidney disease becomes more common as people age.
If a medical condition that affects the kidneys goes untreated, chronic kidney disease generally will worsen over time. Once kidneys have been damaged, it may not be possible to restore the function that's been lost. But if an underlying medical condition is identified and successfully treated, that often will help slow the progression of kidney disease. With some conditions, such as glomerulonephritis, kidney disease can be cured with treatment. This is particularly true when kidney disease is identified in its early stages.
Medication and lifestyle changes, such as losing weight, quitting smoking, and eating less animal protein and salt, also may be necessary to keep kidney disease in check. Fortunately, newer therapies to treat diabetes also may delay progression of kidney failure.
In planning for the future, there is a lot of research underway looking at cell-based therapy, and clinical trials are testing the safety of novel therapies, like stem cells, in patients with chronic kidney disease.
If you have not already done so, I would recommend establishing care with a nephrologist — a physician who specializes in kidney care — as he or she can work with you to identify specific steps and tailored treatment for you to help control your chronic kidney disease — Dr. LaTonya Hickson, Nephrology, Mayo Clinic, Jacksonville, Florida
****************************
Related Articles
- Mayo Clinic Minute: Game-changing treatment for chronic kidney disease could slow down progression of the disease published 3/6/23
- Science Saturday: Seeking a cellular therapy for chronic kidney disease published 11/12/22
- Science Saturday: Mayo Clinic researchers integrate genomics into kidney disease diagnosis, care published 9/17/22
Related Articles







