-
COVID-19
Mayo physician shares diary from a New York COVID ICU
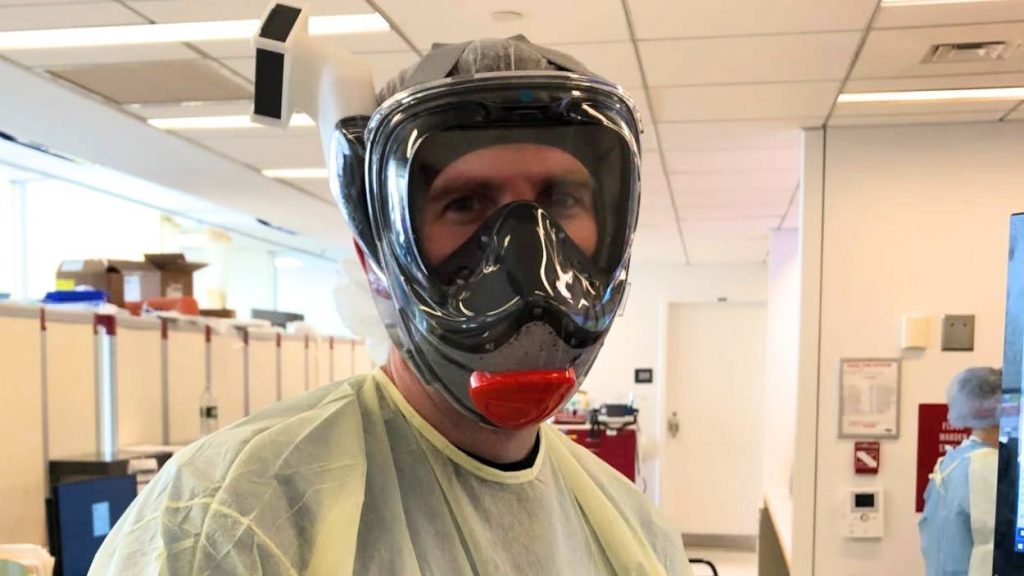
Mayo Clinic intensivist Dr. Ben Daxon saw the effects of COVID-19 up close when he spent a week working in a New York City ICU. He wrote about the experience in "A Doctor's Diary From a COVID ICU."
As a Mayo Clinic intensivist working with the tele-ICU, Ben Daxon, M.D., normally spends his work time in front of computer screens, treating patients remotely. When he learned that a long-time friend was volunteering at a New York City hospital hit hard by COVID-19, he reached out thinking he could help his friend in the same way.
"What my friend described was worse than anything I had heard on the news — much worse," Dr. Daxon writes in an article on TheDispatch.com titled "A Doctor's Diary From a COVID ICU." A third of the health care workers at his hospital were out sick, having contracted the coronavirus themselves. Patients were dying almost every hour and the remaining health care workers didn’t have sufficient equipment.”
While he could have helped remotely, he decided the situation called for helping out in person, and he traveled to New York in April for a one-week assignment at a Brooklyn hospital.
Once the decision was made, he coordinated with the Society of Critical Care Medicine for an assignment, was granted emergency privileges within 24 hours, and had Rochester colleagues offer to cover his shifts. According to an article in The World magazine, he also spent a final night playing with his three children (ages 2, 4 and 6) before leaving. His wife, Amanda, asked him if his will was up-to-date. "We weren’t naïve to how serious this was," she says.
Dr. Daxon supervised an OR recovery area that was converted into an ad-hoc ICU, housing up to 24 patients. It was also the designated hospital for any health care worker who contracted COVID-19. "This way," he says, "people don’t have to take care of their friends or potentially watch them die."
I’m still fresh and eager. Others have been battling this for weeks, and you can see how exhausted and dejected they are. A large part of my role is simply to give them a break.
Ben Daxon, M.D.
In his Dispatch post, Dr. Daxon reflects on his first shift: "As for me, I’m OK. I’m still fresh and eager. Others have been battling this for weeks, and you can see how exhausted and dejected they are. A large part of my role is simply to give them a break."
On his final shift, according to The World magazine article, he noticed a patient’s ventilator was delivering very small breaths. An ultrasound showed that the man had a tear in his lung. His ventilator was still pumping, but the air was trapped. The air pressure could eventually crush the man’s healthy lung and heart. Dr. Daxon had to perform an emergency procedure, inserting needles into the patient’s chest to let the trapped air escape. The patient improved shortly after. It was the first time Dr. Daxon had ever performed the procedure.
Not all of the news was so good. Dr. Daxon says four or five patients died during his volunteer week. After his return home, fortunately, he heard good news about two others: Doctors extubated one patient and discharged the other. "It’s hard to describe to people outside of the ICU how rewarding that is," he says.
He finishes his diary with a hopeful story. "One patient in the ICU had been there over a month," he writes. "She had undergone a surgery with a complicated recovery, but there was no COVID-safe place for her." Her medical team could only hope for the best, though they didn't have much hope. But she made it through without developing COVID-19.
"It’s amazing," he writes. "I don’t want to get into 'commentary creep.' I’m not an epidemiologist nor do I have any expertise in public health policy. But if that patient can make it through a month in the COVID surge ICU, then I think there’s hope for all of us getting through this."
Read more from Dr. Daxon in his post on TheDispatch.com.
This article is written by Mayo Clinic Staff.
Check the Centers for Disease Control and Prevention website for additional updates on COVID-19. For more information and all your COVID-19 coverage, go to the Mayo Clinic News Network and mayoclinic.org.