The Food and Drug Administration has expanded the emergency use authorization for the Pfizer COVID-19 vaccine to include all people 12 and up. To date, about 33 million people in the U.S. have had COVID-19. Mayo Clinic recommends that everyone be vaccinated for COVID-19, even those who were previously infected with COVID-19.
Health experts do not yet know how long you are protected from subsequent infections after recovering from an initial episode of COVID-19. Although infrequent, it is possible that you could be reinfected again, even after you have already recovered from COVID-19.
"Natural immunity to coronaviruses, such as those that cause colds, is not long-lasting, and reinfection is possible," says John O'Horo, M.D., an infectious diseases physician at Mayo Clinic.
"Recent studies have shown that so far COVID-19 induces robust natural immunity for at least one year. This immunity can be substantially boosted with vaccination and provides protection against COVID-19 vaccine variants of concern," says Abinash Virk, M.D., a Mayo Clinic infectious diseases physician. "Additionally, vaccinated persons have demonstrated longer immunity and lower rates of infection than those who were infected, suggesting the vaccines generate a more sustained immunity than natural infection alone."
In addition, the Centers for Disease Control and Prevention has not supported lifting masking restrictions for unvaccinated people.
When to schedule your COVID-19 vaccination
A recent COVID-19 infection could affect the recommended timing of your COVID-19 vaccination.
"We know most people have good short-term immunity following a COVID-19 infection," says Dr. O'Horo, "But studies are showing that those vaccinated shortly after recovery may mount a more robust immune response to the COVID-19 vaccine. This could cause stronger side effects."
All vaccines could cause some degree of reaction. The reason for these side effects is that your immune system is revving up and reacting.
"A 90-day delay is the standard recommendation, but this is not a hard and fast rule. Your situation may call for a shorter delay or a longer delay," says Dr. O'Horo. "If you have had a prior infection, I encourage you to talk with your health care provider about the timing of your COVID-19 vaccination."
Certain treatments and risk factors also can affect the optimal timing for COVID-19 vaccination.
For example, you must delay your COVID-19 vaccination if you meet any of these conditions:
- You are in quarantine from recent COVID-19 exposure.
- You are in isolation from a recent COVID-19 infection or a positive COVID-19 test.
- You received convalescent plasma or monoclonal antibody in the last 90 days.
Health care providers stress that getting vaccinated for COVID-19 is an essential tool in fighting the COVID-19 pandemic. Getting vaccinated can prevent you from getting infected, but more importantly getting vaccinated for COVID-19 can protect you from getting severe infections that can send you to the hospital or require you to be on a ventilator.
____________________________________________
Information in this post was accurate at the time of its posting. Due to the fluid nature of the COVID-19 pandemic, scientific understanding, along with guidelines and recommendations, may have changed since the original publication date.
For more information and all your COVID-19 coverage, go to the Mayo Clinic News Network and mayoclinic.org.
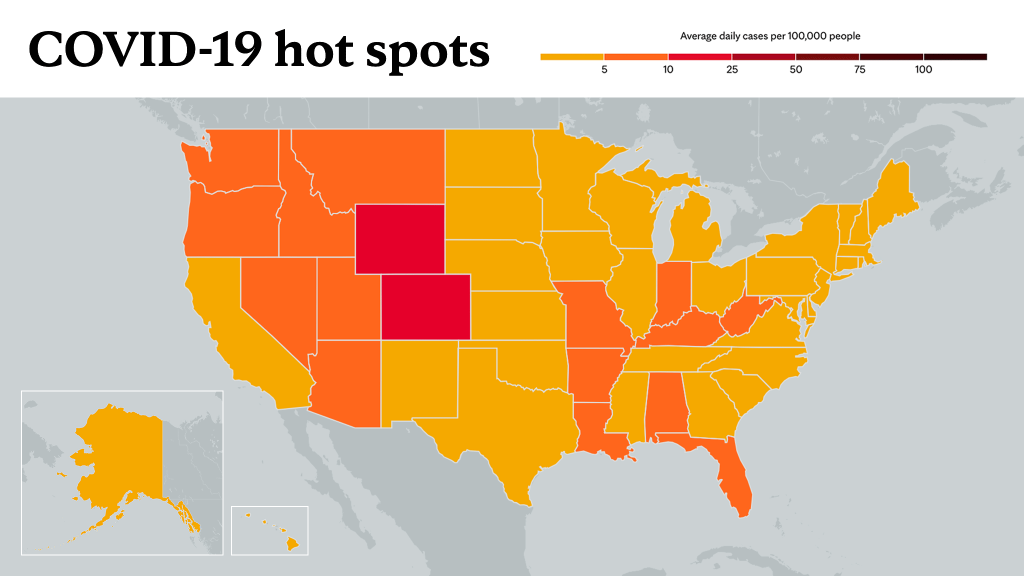
Learn more about tracking COVID-19 and COVID-19 trends.