ROCHESTER, Minn. — Mayo Clinic researchers are taking a close look at rare cases of inflammation of the heart muscle, or myocarditis, in young men who developed symptoms shortly after receiving the second dose of the Moderna or Pfizer messenger RNA (mRNA) COVID-19 vaccines. Several recent studies suggest that health care professionals should watch for hypersensitivity myocarditis as a rare adverse reaction to being vaccinated for COVID-19. However, researchers stress that this awareness should not diminish overall confidence in vaccination during the current pandemic.
While reports of post-vaccine myocarditis in some areas are higher than baseline, the imminent and greater risk for heart damage and death continues to be from becoming infected with COVID-19. Up to 60% of people who are seriously ill with COVID-19 experience injury to their heart, and nearly 1% of fit athletes who had a mild COVID-19 infection show myocarditis on an MRI.
Watch: Dr. Cooper shares more about the connection between myocarditis and the COVID-19 vaccine
Journalists: Broadcast-quality video with Dr. Cooper is in the downloads at the end of the post. Please courtesy: "Mayo Clinic News Network."
A retrospective case series published in JAMA Cardiology studied 23 men in the U.S. military who were hospitalized with myocarditis symptoms within four days of receiving the second dose of a messenger RNA COVID-19 vaccine. Three of the patients previously had been infected with COVID-19, and their symptoms started after the first dose of the vaccine. The cases occurred between January and April. Sixteen had received the Moderna vaccine and seven had received the Pfizer vaccine. For context, it is important to note that the military administered more than 2.8 million doses of messenger RNA COVID-19 vaccines during that time.
All 23 military patients had symptoms of severe chest pain and significantly elevated cardiac troponin levels, which is a protein marker used to measure heart damage. Each patient rapidly recovered, which, combined with the timing and symptoms, supports the diagnosis of hypersensitivity myocarditis. This unusual type of myocarditis is usually related to a drug allergy, but it has been researched in relation to the smallpox vaccine.
"Hypersensitivity myocarditis following vaccination is rare, with the exception of smallpox vaccine. The risk of myocarditis after receiving mRNA vaccine is far less than the risk of myocarditis following actual COVID-19 infection," says Leslie Cooper, M.D., chair of the Department of Cardiology at Mayo Clinic in Florida. Dr. Cooper is senior author of the study, which was conducted with U.S. military medical centers.
Another observational case study recorded details of eight men between the ages of 21 and 56 who were hospitalized with chest pain and diagnosed with myocarditis by laboratory and cardiac MRI. The patients developed symptoms, starting with a fever, within two to four days of receiving their second dose of a COVID-19 vaccine. One patient who had previously recovered from COVID-19 had symptoms after the first dose. All eight patients in the study recovered from the effects of myocarditis and no longer had chest pain. The findings, co-authored by Dr. Cooper with researchers from Mayo Clinic and other medical institutions in the U.S. and Italy, are published in Circulation.
"People of all ages should choose to get a COVID-19 vaccine because the risks are extremely low compared to the benefits. Additionally, the growing body of research shows that vaccine-associated myocarditis resolves quickly in almost all cases," says Dr. Cooper.
###
About Mayo Clinic
Mayo Clinic is a nonprofit organization committed to innovation in clinical practice, education and research, and providing compassion, expertise and answers to everyone who needs healing. Visit the Mayo Clinic News Network for additional Mayo Clinic news. For information on COVID-19, including Mayo Clinic's Coronavirus Map tracking tool, which has 14-day forecasting on COVID-19 trends, visit the Mayo Clinic COVID-19 Resource Center.
Media contact:
- Terri Malloy, Mayo Clinic Public Affairs, newsbureau@mayo.edu
____________________________________________
For the safety of its patients, staff and visitors, Mayo Clinic has strict masking policies in place. Anyone shown without a mask was either recorded prior to COVID-19 or recorded in a nonpatient care area where social distancing and other safety protocols were followed.
Information in this post was accurate at the time of its posting. Due to the fluid nature of the COVID-19 pandemic, scientific understanding, along with guidelines and recommendations, may have changed since the original publication date.
For more information and all your COVID-19 coverage, go to the Mayo Clinic News Network and mayoclinic.org.
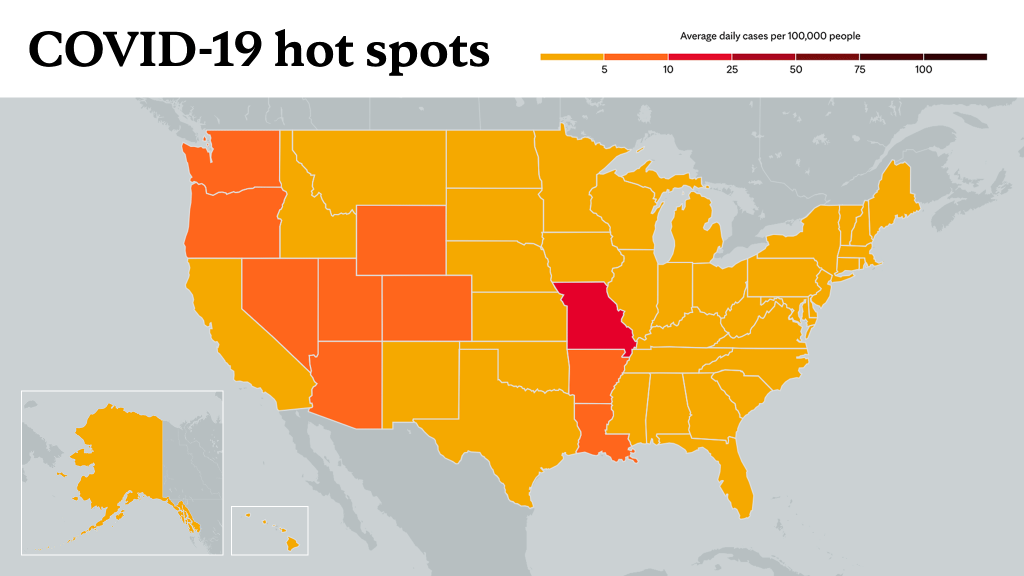
Learn more about tracking COVID-19 and COVID-19 trends.