-
Cardiovascular
Science Saturday: Plasma ceramides – A promising new diagnostic tool for cardiology
Low-density lipoprotein (LDL) cholesterol is the primary measure of atherosclerotic risk and thus a therapeutic target in clinical practice. The focus on LDL cholesterol and its control by diet, lifestyle, and pharmaceuticals has contributed to a significant and sustained reduction in blood concentrations of total and LDL cholesterol among U.S. adults since 1988. Despite population-wide improvements in lipid levels, heart disease remains the No. 1 cause of death both within the U.S. and globally. Consequently, there is an ongoing search for risk factors to help identify and treat patients prior to the development of symptomatic heart disease.
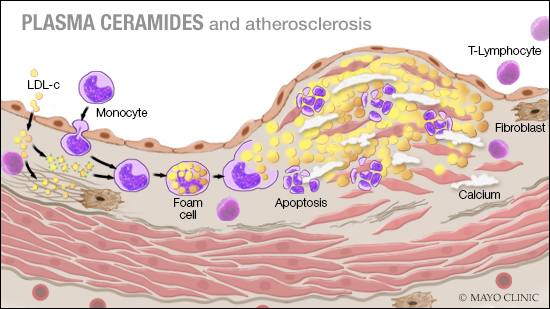
Atherosclerosis begins when lipoproteins infiltrate the vascular intima, drawing monocytes across the endothelium. Phagocytosis of lipoproteins by monocytes creates lipid-bloated foam cells, which release cytokines and effector molecules that promote myocyte migration while upregulating endothelial cell adhesion and platelet activation proteins and disrupting vasodilation mechanisms. Ceramides increase LDL infiltration and promote LDL aggregation (A), are upregulated in response to inflammatory cytokines (B), are enriched in atherosclerotic plaque (C), and increase platelet activation while disrupting endothelial function (D).
Traditional risk factors for atherosclerosis include elevated body mass index, hypertension, smoking, and increased blood cholesterol. Current guidelines endorse focusing on circulating cholesterol and nonspecific inflammatory markers as biomarkers for atherosclerosis. However, the pathophysiology of atherosclerosis is a complex intersection of dyslipidemia, inflammation, endothelial dysfunction, and platelet activation. Recent data support causal associations between each of these pathways and plasma ceramides. Read the rest of the article on Advancing the Science.
___________________________________________
Other Mayo Clinic medical research websites:
- Research at Mayo Clinic
- Discovery’s Edge
- Advancing the Science
- Forefront
- Mayo Clinic Center for Individualized Medicine
- Mayo Clinic Center for Innovation
- Center for Regenerative Medicine
- Center for the Science of Health Care Delivery







