
Eric Salter's life changed unexpectedly in May 2017 when he suffered a life-threatening aortic dissection while working from his home office. The active father of two who was then 42 went from living a normal, healthy life to having just minutes to say goodbye to his family before emergency surgery.
*** NOTE: The Mayo Clinic News Network began telling Eric's story before the COVID-19 pandemic and all video was recorded prior to mask-wearing requirements.
Watch: Specialized heart surgery gives Florida father hope for the future
Journalists: Broadcast-quality video (3:50) is in the downloads at the end of this post. Please "Courtesy: Mayo Clinic News Network." Read the script.
"We thought I was in great shape ― the best shape of my life," says Eric. "I didn't have any symptoms that would tell me that I had this ticking time bomb inside."
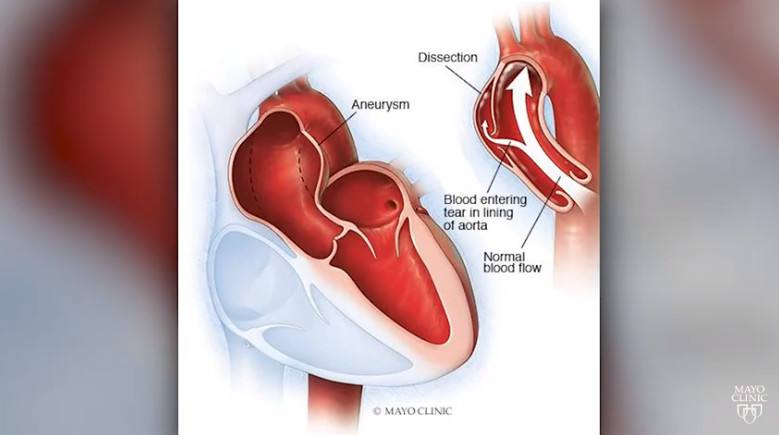
Eric suffered an aortic dissection, which is a tear in the inner layer of the large blood vessel branching off from the heart. He underwent emergency surgery to repair the dissection, which doctors told him had likely been caused by a bicuspid valve issue.
"(After surgery,) I was given the impression that I was 'fixed.' That was a term that was used a lot ― and to go live my life," says Eric.
But after joining an online community for aortic dissection survivors, he and his wife, Madelen Salter, became concerned about the future.
"They were aortic dissection survivors, but they were being told different things and had a different treatment plan than I did," says Eric.
Seven months after his surgery, Eric decided to get a second opinion at Mayo Clinic in Florida. He met with Dr. Sabrina Phillips, a Mayo Clinic cardiologist.
"My initial question to him was, 'Well, when was your last CT scan?' And he told me it was in the hospital," says Dr. Phillips.
"She scheduled a CT scan for me immediately," says Eric.
Dr. Phillips explained that it's important patients like Eric have a follow-up CT scan three months after surgery. Eric's last scan had been more than six months prior.
Eric's scan at Mayo showed that a small outpouching called a "pseudoaneurysm" had developed around the surgical repair site. This outpouching needed to be monitored to make sure it didn't grow over time.
"This is the pseudoaneurysm that grew rapidly, and you can see that the size is almost the size of the aorta. So this is very, very large and was a significant concern for rupture," explains Dr. Phillips.
A rupture could be fatal, so Dr. Phillips advised additional surgery. Because time was of the essence, Eric opted to travel to Mayo Clinic in Rochester, Minnesota, where Dr. Alberto Pochettino, an aortic surgeon, could perform the repair.
Just as Eric and his family were getting back to normal life, he was once again facing a critical surgery.
"It was extremely difficult," says Eric. "Scary, very scary."
In Rochester, Dr. Pochettino performed a complex, 14-hour procedure to fix the immediate area of concern, which included revising the entire ascending aorta graft from Eric's previous surgery.
"Eric did very well with this complicated surgery," says Dr. Phillips, who will continue to monitor Eric's repaired aorta, as more surgery may be required.
"Over time, it is possible that that area of the aorta would expand to a degree that would make it dangerous in terms of risk of rupture. And if that were to occur, we would need to have Eric go back to the operating room for an even more complicated procedure to repair this descending thoracic aorta."
And while Eric says the thought of another surgery is scary, if that time comes, he has faith in Mayo.
"Mayo is where I will go, and I will see Dr. Pochettino for that surgery," says Eric. "And I am confident that they'll do their job."
That confidence is allowing him to focus on the important things in his life and not spend time worrying about the "what ifs."
"I keep reminding myself there are 1,440 minutes in each day. Take advantage of all of them."
__________________________________________________
For the safety of its patients, staff and visitors, Mayo Clinic has strict masking policies in place. Anyone shown without a mask was either recorded prior to COVID-19 or recorded in a nonpatient care area or where social distancing and other safety protocols were followed.








