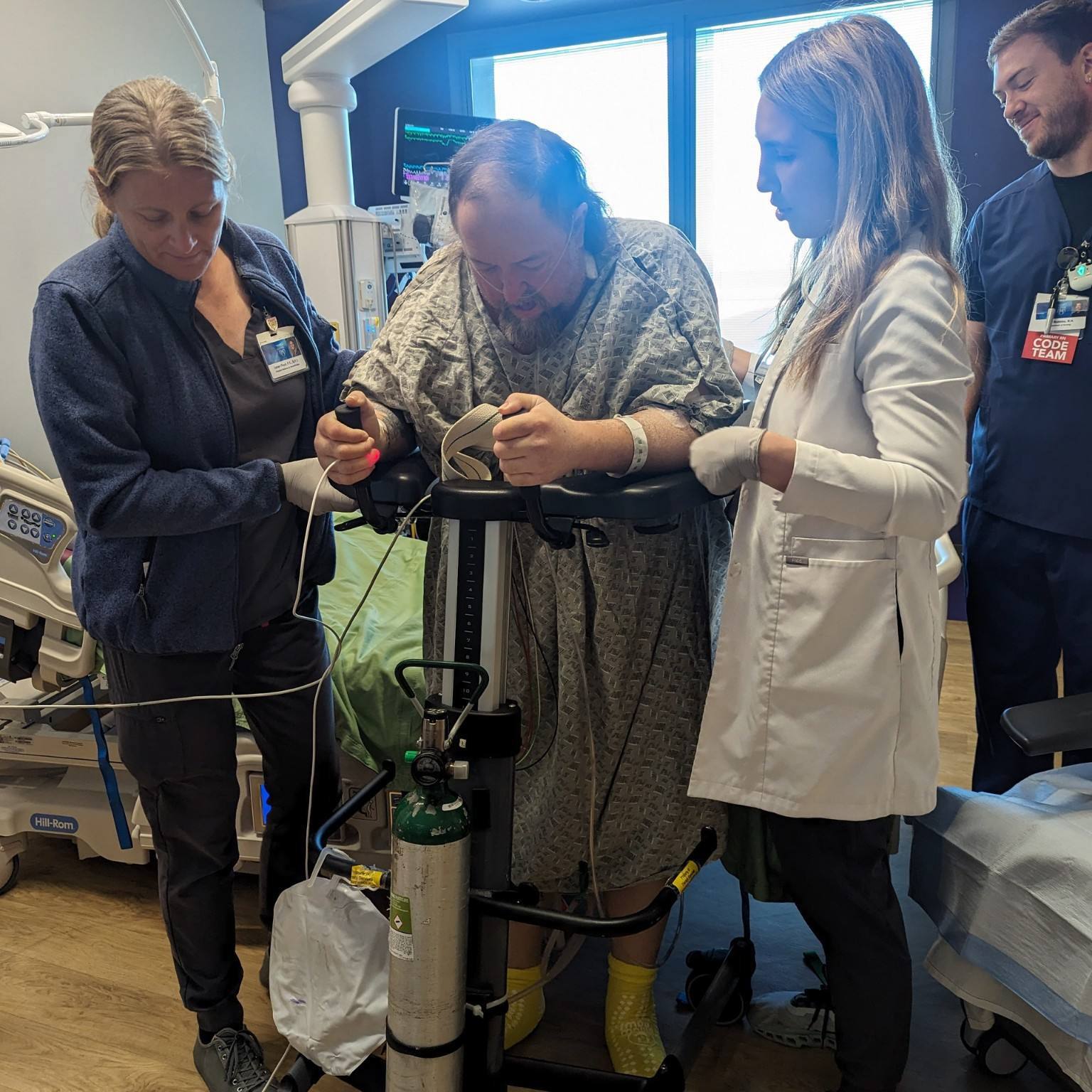
When Mat Walker had a device implanted to aid his failing heart, it was just the beginning of a long road to better health. But a host of Mayo Clinic care providers assembled to assist Mat as he worked toward his recovery goals.
After all he's been through over the past year, Mat Walker takes little for granted. Watching wildlife in his yard, walking to his mailbox and back, and enjoying his meals all mean a little more to the 76-year-old Rice Lake, Wisconsin, man than they did before.
Mat, a retired mechanic, has lived with heart problems since 1989. Through the years, although his heart was failing, the condition was manageable. Medication and regular medical evaluations allowed him to enjoy a normal life with few limitations. He went hunting and fishing, spent time with his family, and worked in his garage.
But in August 2017, Mat's heart failure took a sudden turn for the worse. He felt weak, had trouble breathing, and his legs and ankles swelled to the point that he could hardly get his shoes on. Adjusting his medication didn't work.
Mat spent two weeks under close medical surveillance at Mayo Clinic Health System in Eau Claire, Wisconsin. His condition continued to deteriorate. Mat then was flown to Mayo Clinic's Rochester campus, where his care team would explore whether he was a candidate for a left ventricular assist device, or LVAD. The device is an implantable mechanical pump that moves blood from the lower left side of the heart to the rest of the body.
Fighting for life
The stakes were high for Mat. Nearing the last stage of heart failure, the only alternative to a left ventricular assist device was to return home with hospice care. Neither Mat nor his wife, Sue, were ready for that.
Fortunately, Mat was cleared for open-heart surgery and placement of an LVAD in September 2017. But the struggle wasn't over. Mat came through the surgery; then later he experienced a stroke, blood clot, and gastrointestinal and brain bleeds. He fell into a coma and almost died. The story didn't end there, however. Although it took more than three months in the hospital, Mat recovered.
"He's a fighter and didn't give up," Sue says.
Released from the hospital in December 2017, Mat was still too weak to go home. He was transferred to Mayo Post Acute Care in Barron, Wisconsin, where he received speech therapy twice a day, along with occupational and physical therapy. Because he had breathing and feeding tubes in place for so long, the muscles in his throat needed time to recover. It took seven months for him to be able to eat through his mouth again.
Mat went home in February 2018 with the assistance of home health services from Mayo Clinic Health System. His team included a skilled nurse, physical therapist, occupational therapist, speech-language pathologist and dietitian. Together, they developed a plan of care to help him recover and return to a maximum level of function.
"They had quite the team. I felt like anytime I needed someone to talk to, I could call 24/7."
Sue Walker
"They were great. I can't emphasize that enough," says Sue, recalling how much more comfortable she felt bringing her husband home with home care in their corner. "They had quite the team. I felt like anytime I needed someone to talk to, I could call 24/7."
Amy S. Anderson, a physical therapist with Mayo's Home Health and Hospice, worked with Mat for six months. Initially, he was weak and his mobility was extremely limited. He required assistance to get up from a chair, get into bed and walk down the hall. The team set step-by-step goals, and Mat began to progress. The improvements were small at first, such as getting up out of a chair with his wife by his side but not helping him. Over time, they became larger, such as when Mat began walking independently up and down the four steps to get in and out of his home.
Most people receive home care services for less than two months, but Mat required more recovery time than that. Anderson marvels at how far he's come.
"At first when we met him, he was quite weak and unsure of himself," she says. "He was very focused on his limitations versus his abilities and couldn't see the light at the end of the tunnel. As we started working with him, you could see him gaining confidence."
Returning to beloved pastimes
One of Mat's biggest goals was to once again be able to spend time in his garage where he kept his tools and an old car.
"We could just see the light come on when, all of the sudden, he could walk down the steps and do something that was extremely important to him," Anderson says.
Mat remembers little from the ordeal, but he says he feels "great, just super" today. He still uses a walker in the house for balance but is doing well overall. He says words can't express the gratitude he feels toward his medical team for getting him through his crisis and back onto his feet.
"Out of all the patients we see, this story will always stick out in my mind."
Amy S. Anderson
Sue, who remembers every frightening step in vivid detail, also is extremely appreciative. "I just want to thank all the doctors and nurses that helped Mat through this and, of course, the LVAD team," she says. "He's just happy to be home and enjoying life."
For Anderson, playing a part in Mat's rehabilitation was a rewarding experience.
"You always hear about the collaboration of Mayo Clinic. Truly — between surgery in Rochester and Mayo Post Acute Care in Barron, his visits to the Cardiac Center in Eau Claire, home care visits, going to outpatient physical therapy at Mayo Clinic Health System in Rice Lake — you can really see how we all worked together in transitioning his care to the most appropriate level at any given time," Anderson says. "Out of all the patients we see, this story will always stick out in my mind."
Note: A version of this story previously was published in Hometown Health.
HELPFUL LINKS
- Learn more about ventricular assist devices.
- Read about Mayo Post Acute Care.
- Connect with others talking about cardiovascular conditions on Mayo Clinic Connect.
- Explore Mayo Clinic Health System.
- Request an appointment.
Related Articles