-
Women’s Wellness: Why can’t I poop?

This article is written by physical therapist Laura Meihofer for Mayo Clinic's Office of Women's Health.
Do you find yourself sitting on the toilet for long periods of time? Do you rely upon over the counter stool softeners, laxatives or fiber to have a bowel movement? Is passing a bowel movement painful, or do you find yourself straining excessively to fully empty your bowels? You may be suffering from constipation, the most common gastrointestinal complaint affecting 42 million Americans (1). Constipation is often the result of multiple contributing factors. After seeing your local healthcare provider to assess the problem, a visit to a physical therapist specializing in pelvic floor health may be useful.
You may be thinking, “Why a physical therapist? I thought they only looked at my neck, shoulders or back.” A physical therapist specializing in pelvic floor health has been specifically trained to assess not only your back, but also your boney pelvis and hips which may be contributing to your constipation. He or she is also trained to assess the impact of various behaviors, medications and diseases on the pelvic floor as well as to examine the pelvic floor muscles specifically. The pelvic floor is a group of muscles that forms a bowl in your pelvis. This muscle group must contract, relax, and most importantly, coordinate between these two motions to maintain continence of stool and urine and allow you to pass a bowel movement or urinate at will (2).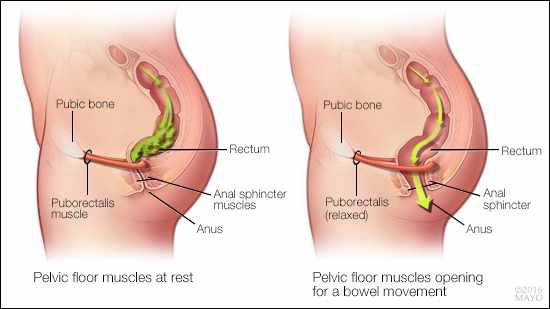
When you visit a pelvic floor physical therapist for constipation, he or she will first ask you about various aspects of your bowel health. These questions may include how long you have experienced constipation, which medications (prescribed or over-the-counter) are you taking, how much fluid you are consuming, and what your activity level is. The therapist may also want to know the consistency (soft, smooth, hard, or lumpy) and frequency of your bowel movements and whether you experience pain in your abdomen or rectum with passage of a bowel movement, excessive straining or a sense of not fully emptying your bowels.
After reviewing your history, the therapist will evaluate the pelvic floor muscles by looking at the pelvic floor and observing how it moves when you breathe, relax or contract, for example. He or she might ask you to tighten your muscles as if you were stopping the flow of urine or to relax the muscles by bearing down as if you were pushing something out. The therapist may also gently palpate the pelvic floor muscles to see if they are tight and tender or soft and supple. Depending on the situation and your comfort level, the therapist might also complete an internal assessment of the pelvic floor muscles checking for tightness or tenderness and evaluating your control over these muscles.
After understanding your concerns, taking a history and performing a physical examination, your therapist will develop a treatment plan specific to your needs. This treatment plan might be carried out over several sessions and may include hands-on techniques to aid in muscle relaxation and to improve muscle awareness as well as behavioral modification (drinking more fluid, for example) and exercises to help improve your pelvic floor health (3, 4).
If you are suffering from constipation or pain with bowel movements, excessive straining, or relying upon medication to have a bowel movement, pelvic floor physical therapy may be the answer for you. To find a pelvic floor physical therapist in your area visit the American Physical Therapy Association Section on Women’s Health.
###
Higgins PD, Johanson JF. Epidemiology of constipation in North America: a systematic review. American Journal of Gastroenterology. 2004;99:750–759.
Recognition and Management of Nonrelaxing Pelvic Floor Dysfunction Stephanie S. Faubion, MD Lynne T. Shuster, MD Adil E. Bharucha, MBBS, MD
Collins, E., Hibberts, F., Lyons M., Williams, A. B., & Schizas, A. P. (2014). Outcomes in non-surgical management for bowel dysfunction. British Journal of Nursing, 23(14), 776-780. Doi:10. 12968/bjon.2014.23.14.776
Successful physical therapy for constipation related to puborectalis dyssynergia improves symptom severity and quality of life. Lewicky-Gaupp C; Morgan DM; Chey WD; Muellerleile P; Fenner DE. Diseases of the Colon & Rectum. 51(11):1686-91, 2008 Nov.