-
 Minnesota
MinnesotaMayo Clinic Health Letter: Highlights from the July 2014 Issue
ROCHESTER, Minn. ― Here are highlights from the July issue of Mayo Clinic Health Letter. You may cite this publication as often as you wish. Reprinting is allowed for a fee. Mayo Clinic Health Letter attribution is required.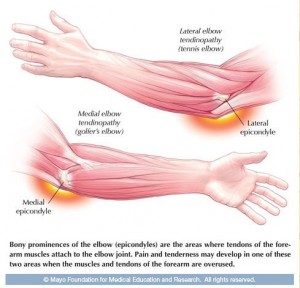 Include the following subscription information as your editorial policies permit: Visit www.HealthLetter.MayoClinic.com or call toll-free for subscription information, 1-800-333-9037, extension 9771. Full newsletter text: Mayo Clinic Health Letter July 2014 (for journalists only).
Include the following subscription information as your editorial policies permit: Visit www.HealthLetter.MayoClinic.com or call toll-free for subscription information, 1-800-333-9037, extension 9771. Full newsletter text: Mayo Clinic Health Letter July 2014 (for journalists only).
Elbow pain: Quicker recovery with a health care provider
When elbow pain stops golf, tennis, gardening or household chores, it’s wise to see a doctor to determine the cause and a treatment plan. The July issue of Mayo Clinic Health Letter covers common causes of elbow pain, self-care tips and why seeing a doctor sooner ― rather than later ― is a good idea.
In the absence of a bone fracture, most elbow injuries aren’t serious. But nagging pain can interfere with sports and day-to-day activities. Most elbow pain is related to overuse that results in irritation and tissue degeneration near areas where tendons connect to bones of the elbow joint.
When pain occurs on the outside of the elbow, it’s called lateral elbow tendinopathy ― or tennis elbow. When pain occurs on the inside of the elbow, it’s called medial elbow tendinopathy ― or golfer’s elbow. They share some symptoms, including a dull aching or burning feeling in the elbow area when at rest. Use of the forearm is the primary cause of sharper pain. Gripping or forearm-twisting motions such as lifting objects palm down, shaking hands or turning a doorknob also can cause pain.
Rest and self-care may lead to healing over time. But it’s generally true that recovery will be quicker when working with a doctor or physical therapist to develop a treatment plan specific to the cause of the pain. The treatment plan may include stretching and strengthening exercises, application of therapeutic ultrasound energy or mild electrical current. Other treatment options are available, too, ranging from injections of corticosteroids to surgery.
Once pain has developed, self-care steps include:
Avoiding or modifying activities: Avoid activities that cause pain. Minimizing aggravation may help reduce the length of recovery time. If the pain is due to tennis or golf, instruction in proper technique can help ensure that the swing comes from large muscles and not the wrist and forearm.
Ice and pain control: Icing the area for 15 minutes three or four times a day may reduce pain. Ordinary nonprescription pain medications may help reduce pain but don’t aid in healing.
Gentle stretching: Moving the elbow and wrist through the full range of motion and gentle stretching of the wrist in an up or down position can help.
Loneliness ― A surprising health risk
Despite advances in technology that allow for new ways to connect, evidence suggests that loneliness is more common than ever. When loneliness persists, it can have profound effects on the body, according to the July issue of Mayo Clinic Health Letter.
Research suggests that the effects of loneliness may be worse than carrying around extra pounds ― increasing the chances of premature death by 14 percent. It may not be surprising that loneliness affects mental health and often goes hand in hand with depression. But the effects can be much broader. One recent study associated loneliness with an increased risk of developing dementia later in life. Another showed that lonely people are subjected to fragmented sleep, a factor that’s significant due to the profound impact of quality sleep on health.
Loneliness need not be a chronic condition, but renewing and making connections takes effort and stepping out of one’s comfort zone.
Mayo Clinic Health Letter offers these suggestions to nurture friendships and make new ones:
Reach out: An unexpected phone call, even just to say hello, is a meaningful gesture.
Be positive: Think of friendship as an emotional bank account. Make deposits of kindness and approval, keeping in mind that criticism and negativity draw down on the account.
Extend and accept invitations: Invite a friend for coffee or lunch. Accept invitations to social gatherings.
Participate in community events: Join with a group of people working toward a mutual goal ― winning an election or cleaning up a park.
Take up a new interest: Join a class at a gym, senior center or community fitness facility.
Take a walk: Chat with neighbors who are out and about or head to a park and strike up a conversation.
Think beyond two legs: Whether it has four legs or even wings, a pet can provide many of the same companionship benefits as humans.
It’s important to not confuse loneliness with being alone. A solid support system makes it easier to navigate alone times with ease or even pleasure.
Magnetic stimulation can improve hard-to-treat depression
Transcranial magnetic stimulation (TMS) ― using brief, powerful electromagnetic pulses to alter pathways in the brain ― is a new option for treating depression that hasn’t responded to standard therapy. The July issue of Mayo Clinic Health Letter covers TMS, its effectiveness and what types of patients might benefit from this therapy.
Depression often is successfully treated with antidepressant medications in combination with counseling. But for about 20 percent of those with depression, drugs may not be well tolerated or may not have enough of an effect to cause remission of the disease. The Food and Drug Administration has approved TMS for use in those who have completed an unsuccessful trial of antidepressant medications and counseling.
During TMS, patients remain awake and alert as the magnetic pulses are applied. Treatment doesn’t interfere with the ability to drive or work. And unlike electroconvulsive therapy, another option for hard-to-treat depression, it is not intended to cause seizures and doesn’t cause memory problems.
TMS requires an investment of time. A typical appointment lasts about an hour. Therapy is administered five days a week for four to six weeks. Sticking with the schedule is important, as the benefits may not fully emerge until late in the course of therapy. TMS therapy may not be covered by insurance.
Studies have shown some symptom-reducing effects in 50 to 60 percent of people who undergo TMS, and the treatment leads to remission of depression symptoms in about 30 to 40 percent of people.
Some maintenance therapy is typically performed after successful TMS therapy. Most often, treatment is an antidepressant medication along with counseling. One study that looked at the durability of TMS treatment found that about 52 percent of study participants held their improvement with maintenance therapy of a single antidepressant medication and counseling. About 38 percent had symptoms worsen, but most regained remission with additional TMS sessions. About 10 percent of study participants had a relapse of depression symptoms.
Research is underway to determine possible changes to TMS delivery that may improve outcomes.
###
Mayo Clinic Health Letter is an eight-page monthly newsletter of reliable, accurate and practical information on today’s health and medical news. To subscribe, please call 1-800-333-9037 (toll-free), extension 9771, or visit www.HealthLetter.MayoClinic.com.
About Mayo Clinic
Recognizing 150 years of serving humanity in 2014, Mayo Clinic is a nonprofit worldwide leader in medical care, research and education for people from all walks of life. For more information, visit 150years.mayoclinic.org, www.mayoclinic.org and newsnetwork.mayoclinic.org.
MEDIA CONTACT: Brian Kilen, Mayo Clinic Public Affairs, 507-284-5005, newsbureau@mayo.edu