-
Lewy Body Dementia: Unfamiliar With This Common Disorder?
International conference Dec. 1 – 4 brings together experts, patients and caregivers
ROCHESTER, Minn. — Lewy body dementia is the second most common type of dementia after Alzheimer’s disease. But if you’re not familiar with it, you’re not alone. “Lewy body dementia is the most common disorder you’ve never heard of,” says Bradley Boeve, M.D., a Mayo Clinic neurologist who will speak at the International Dementia with Lewy Bodies Conference Dec. 1-4 in Fort Lauderdale, Florida.
Lewy body dementia shares similar symptoms of memory issues like Alzheimer’s and slow, stiff movements like Parkinson’s disease. But people with Lewy body dementia may act out their dreams while asleep, or they may have visual hallucinations that can lead to unusual behavior, such as having conversations with deceased loved ones.
Getting an accurate diagnosis is the key to improving patients’ lives, says Dr. Boeve, co-investigator of the Mayo Clinic Dorothy and Harry T. Mangurian Jr. Lewy Body Dementia Program. “We want to help patients stop the diagnostic odyssey of seeing many different clinicians, undergoing many different tests over an extended period of time with no clear answers and all of the frustration that goes with this,” Dr. Boeve says.
Journalists: Sounds bites with Dr. Boeve are available in the downloads.
For an interview with Dr. Boeve, contact Susan Barber Lindquist at 507-284-5005 or newsbureau@mayo.edu.
While there’s no cure today for Lewy body dementia, an accurate diagnosis can help patients receive the right medications. Some medications that don’t work for Alzheimer’s may help improve Lewy body dementia symptoms.
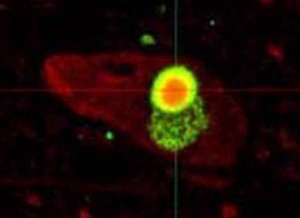
Dr. Boeve explains it this way: In Lewy body dementia, protein deposits – named after Frederick Lewy who discovered them — develop in brain cells. While some brain cells die, others are just not working properly. Certain medications, called cholinesterase inhibitors, help trigger nerve impulses from one brain cell to the next — sometimes improving symptoms.
Lewy body dementia symptoms include:
- Visual hallucinations: Seeing colors, shapes, animals or people that aren’t there.
- Movement disorders: Slowed movement, rigid muscles, tremors or shuffling walk.
- Poor regulations of body function: Dizziness, falls and bowel issues.
- Cognitive problems: Confusion, reduced attention span and memory loss.
- Sleep difficulties: Physically acting out dreams while asleep.
- Fluctuating attention: Drowsiness, staring into space, daytime naps and disorganized speech.
- Depression: Persistent sadness and loss of interest.
While the cause of Lewy body dementia is unclear, risk factors include being older than 60, being male and having a family member with Lewy body dementia.
After diagnosis, doctors, patients and caregivers work together to monitor medications and find nondrug approaches.
“Education and empowerment of patients and families are critical,” Dr. Boeve says. “For example, if visual hallucinations are present, learning techniques to manage them can help avoid Emergency Department visits or hospitalizations, so it’s cost saving and lessens patients’ and families’ frustration. The education and support by the Lewy Body Dementia Association are also critical.”
The International Dementia with Lewy Bodies Conference includes sessions for health care providers, patients and caregivers. Dr. Boeve and his colleagues in Mayo Clinic’s Lewy Body Dementia Research Program are the hosts, working in conjunction with the staff of the Lewy Body Dementia Association.







