-
Mayo Clinic Minute: Improving bone health before spinal surgery
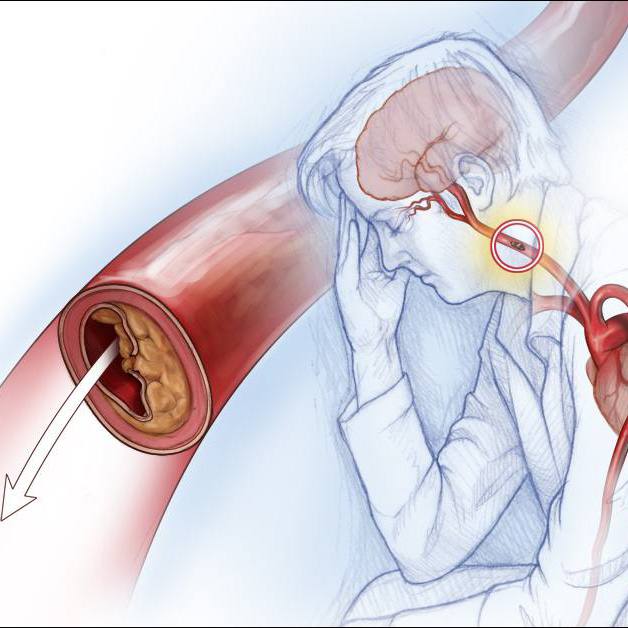
As people age, bones lose some of their structure. Osteopenia and osteoporosis are both conditions in which bones become less dense and, therefore, can break more easily. These kinds of bone density issues are common among spinal surgery patients who are 50 and older. To avoid surgical complications, Mayo Clinic works with these patients on improving bone health before spinal surgery.
Journalists: Broadcast-quality video (1:07) is in the downloads at the end of this post. Please courtesy: "Mayo Clinic News Network." Read the script.
Making sure a patient's bones are as healthy as possible before undergoing spinal surgery has been shown to lower the rate of complications.
"These are already high-risk surgeries. And so we want to get the risks as low as possible before proceeding," says Dr. Benjamin Elder, a Mayo Clinic neurosurgeon.
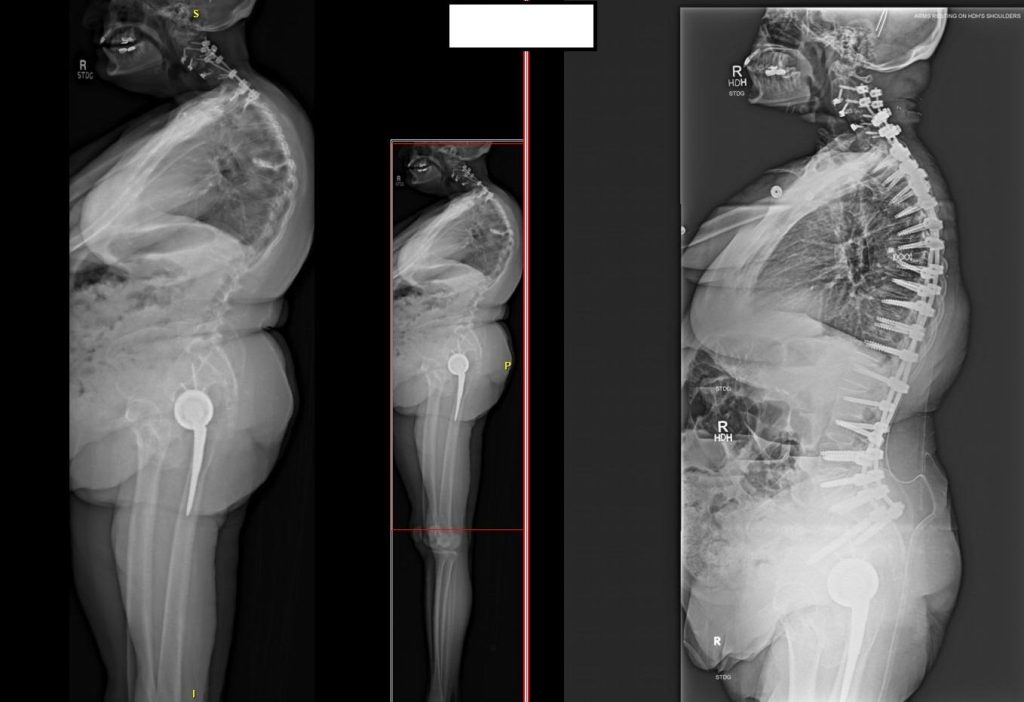
Dr. Elder says some adult deformity surgery as well as reconstructive and revision surgeries involve attaching screws or other hardware to strengthen and stabilize the spine.
"If you think about putting a screw into drywall or into a stud, there's a big difference. And so some of the patients with severe bone density issues or severe osteoporosis, their bone is not even drywall, it's kind of the paper on the drywall. So if we put screws into it, they'll pull out immediately," he says.
Mayo Clinic neurosurgeons and endocrinologists, who specialize in bone metabolism, work together to help patients improve bone mineral density before spinal surgery.
The bone-strengthening therapy can include medications that help build bone back up, as well as implementing lifestyle changes.
"Before any sort of our spine fusion surgeries, we make patients stop all nicotine use, as that has a significant decline in the fusion rate. And it can also have effects on wound healing," says Dr. Elder.
Related Articles