-
Featured News
Mayo Clinic Q and A: Dysphagia is a common concern with several possible explanations
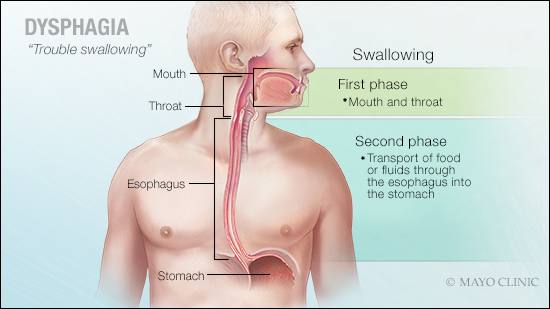
DEAR MAYO CLINIC: My mother is in her 80s and sometimes has trouble swallowing when she’s eating. She says it’s not bothering her much, but I feel like it’s starting to affect how much and how often she eats. Is there anything that can be done to treat this problem?
ANSWER: It’s likely your mother’s problem with swallowing can be better understood and potentially helped, but it will require a medical evaluation. Having difficulty swallowing is a common concern that has several possible explanations. A thorough assessment of your mother’s condition can uncover the cause and guide treatment.
When a person is having trouble swallowing — the medical term is dysphagia — the first step is to identify the point in the swallowing process where the problem is happening. There are two phases of swallowing. The first is the oropharyngeal phase. It involves the mouth and throat. The second is the esophageal phase. It involves the transport of food or fluids from the throat into the stomach through the esophagus (food pipe). Determining whether swallowing difficulty is related to oropharyngeal transfer or esophageal transit often can be accomplished by reviewing the symptoms people experience when they swallow.
The oropharyngeal phase requires proper function of muscles in the palate, as well as appropriate tongue motion and airway protection during swallowing. That all happens in a coordinated sequence that allows for smooth transit of food and fluid from the mouth, through the throat and into the top of the esophagus.
With oropharyngeal issues, patients typically begin to choke, cough or gag almost immediately after attempting to swallow. Material may come out the nose or slip out of the mouth. If an oropharyngeal problem is suspected, a health care provider may ask a patient to drink some water so the provider can observe what happens. Conditions that cause oropharyngeal swallowing difficulties include many neurological diseases, such as stroke and Parkinson’s disease.
In the esophageal phase, the muscles of the esophagus have to contract and relax in a coordinated fashion to move food to the stomach. The passageway within the esophagus also needs to be wide enough to allow food through it easily.
If the problem is related to esophageal transit, the material clears the patient’s mouth and throat without incident, and he or she can breathe easily. But the patient feels as if something is stuck behind the breastbone or there is pain in the esophagus while swallowing. Eventually what was swallowed will typically pass, but in some cases the material is regurgitated.
When an oropharyngeal problem seems to be the cause, a pharyngeal swallowing study typically is performed with X-rays. This study can reveal structural issues, or problems with muscle coordination or strength in the mouth or throat.
If it appears to be an esophageal concern, the first test usually is endoscopy. During this procedure, a thin, flexible and lighted instrument, called an endoscope, is passed down the throat, so the doctor can see into the esophagus to check for blockages, narrowing, inflammation or other structural issues. In some cases, tissue samples may be taken. If narrowing of the esophagus is found, expansion of the esophagus may be performed during an endoscopy, too.
When results of an endoscopy are normal, the focus shifts to a possible esophageal motility problem or muscle dysfunction, although generally these disorders are uncommon. An esophageal muscle test, called “manometry,” can be used to measure muscle contractions in the esophagus.
Specific treatment for swallowing difficulty depends on the underlying cause. In most cases, however, problems with swallowing can be relieved or significantly reduced once the source is identified.
It is important have the problem addressed. Not only can swallowing difficulty interfere with nutrition and potentially trigger unhealthy weight loss, but also it can cause quality of life issues. Some people who have swallowing difficulty are embarrassed by it and avoid socializing in settings that involve food. That can lead to social isolation and potentially depression. Encourage your mother to see her health care provider for an evaluation soon. — Dr. Magnus Halland, Gastroenterology and Hepatology, Mayo Clinic, Rochester, Minnesota