-
Featured News
Mayo Clinic Q and A: Hashimoto’s thyroiditis — will diet alone help?
DEAR MAYO CLINIC: I just turned 30 and recently was diagnosed with Hashimoto’s thyroiditis. I’m wondering about whether it can be cured or if I will have to take medication for the rest of my life. I’ve read the Autoimmune Protocol (AIP) diet may help. Is this true? Do you have any suggestions for managing symptoms?
ANSWER: Hashimoto’s thyroiditis is an autoimmune condition that usually progresses slowly and often leads to low thyroid hormone levels — a condition called hypothyroidism. The best therapy for Hashimoto’s thyroiditis is to normalize thyroid hormone levels with medication. A balanced diet and other healthy lifestyle choices may help when you have Hashimoto’s, but a specific diet alone is unlikely to reverse the changes caused by the disease.
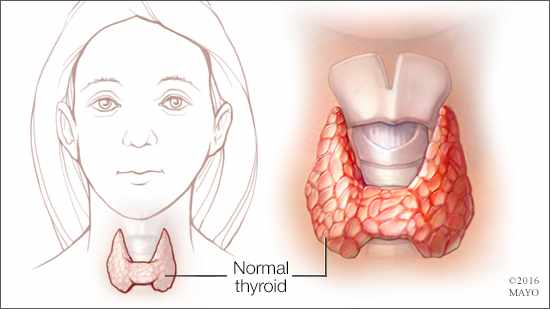
Your thyroid is a small, butterfly-shaped gland at the base of the front of your neck. The hormones that the thyroid gland makes — triiodothyronine (T3) and thyroxine (T4) — affect all aspects of your metabolism. They maintain the rate at which your body uses fats and carbohydrates, help control your body temperature, influence your heart rate, and help regulate the production of proteins.
Hashimoto’s thyroiditis develops when your body’s immune system mistakenly attacks your thyroid. It’s not clear why this happens. Some research seems to indicate that a virus or bacterium might trigger the immune response. It’s possible that a genetic predisposition also may be involved in the development of this autoimmune disorder.
A chronic condition that develops over time, Hashimoto’s thyroiditis damages the thyroid and eventually can cause hypothyroidism. That means your thyroid no longer produces enough of the hormones it usually makes. If that happens, it can lead to symptoms such as fatigue, sluggishness, constipation, unexplained weight gain, increased sensitivity to cold, joint pain or stiffness, and muscle weakness.
If you have symptoms of hypothyroidism, the most effective way to control them is to take a hormone replacement. That typically involves daily use of a synthetic thyroid hormone called levothyroxine that you take as an oral medication. It is identical to thyroxine, the natural version of a hormone made by your thyroid gland. The medication restores your hormone levels to normal and eliminates hypothyroidism symptoms.
You may hear about products that contain a form of thyroid hormones derived from animals. They often are marketed as being natural. Because they are from animals, however, they aren’t natural to the human body, and they potentially can cause health problems. The American Thyroid Association’s hypothyroidism guidelines recommend against using these products as a first-line treatment for hypothyroidism.
Although hormone replacement therapy is effective at controlling symptoms of Hashimoto’s thyroiditis, it is not a cure. You need to keep taking the medication to keep symptoms at bay. Treatment is usually lifelong. To make sure you get the right amount of hormone replacement for your body, you must have your hormone levels checked with a blood test once or twice a year.
If symptoms linger despite hormone replacement therapy, you may need to have the dose of medication you take each day adjusted. If symptoms persist despite evidence of adequate hormone replacement therapy, it’s possible those symptoms could be a result of something other than Hashimoto’s thyroiditis. Talk to your health care provider about any bothersome symptoms you have while taking hormone replacement therapy.
A healthy lifestyle that includes eating well, getting plenty of sleep, exercising regularly and limiting stress can benefit your immune system, and could contribute to an improvement in your immune health. However, there’s no evidence that following one diet in particular is an effective treatment for autoimmune disorders such as Hashimoto’s thyroiditis. If you have questions about diet or other lifestyle choices you can make to improve your health when you have Hashimoto’s, please talk to your doctor. — Dr. Victor Bernet, Endocrinology, Mayo Clinic, Jacksonville, Florida