-
Health & Wellness
Mayo Clinic Q and A: What is sarcoidosis?
DEAR MAYO CLINIC: I recently was diagnosed with sarcoidosis, but I don’t currently have symptoms. What causes sarcoidosis? Could it go away on its own? What should I be on the lookout for as far as symptoms that may develop?
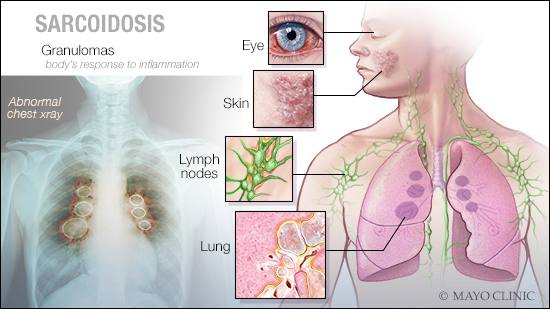
ANSWER: Sarcoidosis is an inflammatory disease characterized by the formation of tiny collections of inflammatory cells called “granulomas.” These granulomas can deposit in any part of the body and affect almost any organ, but the most commonly affected areas are the lungs, lymph nodes, eyes and skin. Experts believe the condition happens as a result of the body’s immune system responding abnormally to an unknown substance in the environment. Sarcoidosis is thought to occur in people who have a specific genetic predisposition. While sarcoidosis sometimes runs in families, it is not considered a hereditary disease. It also is not contagious.
Sarcoidosis can develop suddenly and present with acute symptoms, or develop gradually over months or years. However, many times sarcoidosis does not cause any symptoms and is found during a routine follow-up or evaluation of some other condition.
When symptomatic, sarcoidosis may cause general symptoms such as fatigue, fever, swollen lymph nodes and weight loss. Other signs and symptoms would vary, depending on which organs are affected. The most common presenting symptoms that may trigger an evaluation for sarcoidosis include shortness of breath; persistent dry cough; wheezing; chest pain; red eye or vision problems; discoloration of the nose, cheeks, lip and ears; skin rash; joint pain; and irregular heartbeat.
Sarcoidosis sometimes is difficult to diagnose, as it can mimic other diseases. For that reason, your health care provider may recommend performing several tests, depending on your specific symptoms, before he or she can establish a final diagnosis. Commonly, a chest X-ray, an EKG, blood work and a breathing test are recommended as part of the initial evaluation. In some cases, a biopsy of the area believed to be affected is used to identify the presence of the granulomas and provide further evidence toward the diagnosis.
Once the diagnosis is made, if your lungs are normal or have minimal changes, but you do not have other symptoms, your health care provider may not recommend any treatment — even if granulomas are found in your biopsy.
Follow-up care is recommended, however, for most people, but the frequency will be based on symptoms, and a person’s overall health and situation. Sarcoidosis monitoring typically includes regular chest X-rays, and examinations of the eyes, skin and any other organs that might be affected by the disease. But talk to your health care provider about the schedule recommended for you.
If you start to develop respiratory problems, such as shortness of breath, persistent cough or abnormal breathing, palpitations, chest pain, visual problems, weakness, or numbness, contact your health care provider right away. You may need tests to see if the disease activity has changed. Any specific treatments would depend on that assessment.
Although there is no cure for sarcoidosis, it is common for the disease to go away on its own without treatment or with minimal treatment to manage symptoms. That said, its signs and symptoms may persist long term. In severe cases, sarcoidosis can lead to organ damage.
Because sarcoidosis may worsen, it is important that you have regular checkups with your health care provider to monitor your condition and make a treatment plan if symptoms appear. If you notice new symptoms or have other changes in your health, contact your health care provider as soon as possible to see if you need additional evaluation. — Dr. Eva Carmona Porquera, Pulmonary and Critical Care Medicine, Mayo Clinic, Rochester, Minnesota
****************************
Related Articles
- Science Saturday: A hard look at a devastating heart disease published 2/2/19
Related Articles







