-
Infectious Diseases
West Nile virus cases reported across the US
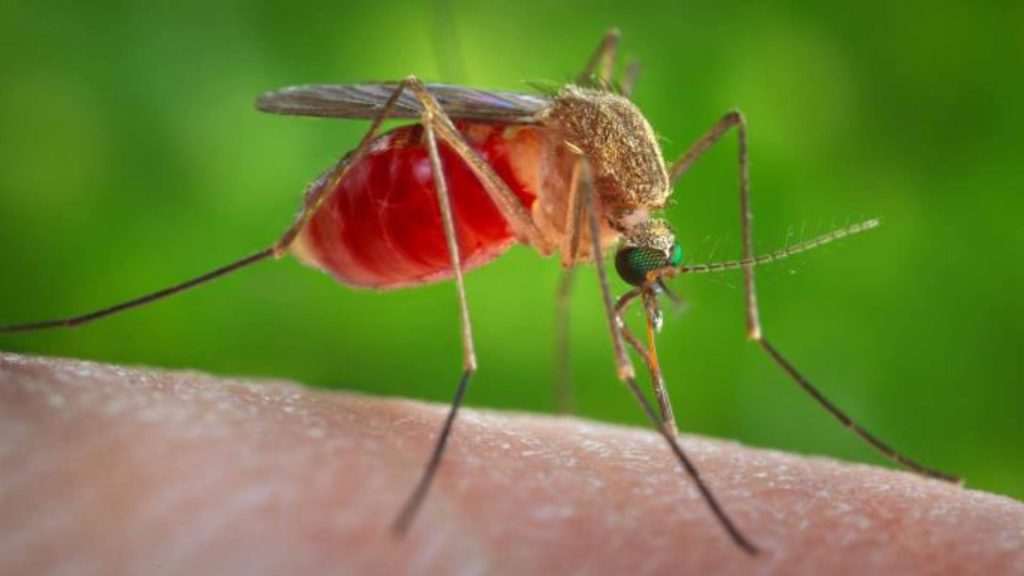
Cases of West Nile virus, a mosquito-borne illness, have been reported across the U.S. It's the leading cause of mosquito-borne disease in the continental U.S., according to the Centers for Disease Control and Prevention (CDC).
"We are currently seeing high levels of West Nile virus infection across many parts of the United States, including a higher number than normal of people with neuroinvasive disease ― the most severe form of infection," says Dr. Bobbi Pritt, director of the Clinical Parasitology Laboratory in Mayo Clinic's Department of Laboratory Medicine and Pathology. "In neuroinvasive disease, the brain and surrounding tissues become inflamed, resulting in permanent brain damage and even death. Approximately 1 in 10 people with neuroinvasive disease die, and those who survive are often left with permanent disabilities."
So far this year, 210 cases of West Nile virus have been reported in humans, with 65% being cases of neuroinvasive disease, according to the CDC.
"That is significantly higher than what we usually see, in which only about 1 in 150 people with West Nile virus disease develop neuroinvasive disease. However, we need to be cautious in interpreting the statistics, since many of the West Nile virus cases without involvement brain involvement may be underdiagnosed. The states with the highest number of neuroinvasive disease cases so far this year are South Dakota, North Dakota, Nebraska, Colorado and Arizona," Dr. Pritt says.
The virus was first isolated in the Nile district in Uganda in 1937. Now the largest outbreaks are reported to be in Greece, Israel, Romania, Russia and the U.S.
"It swept through the U.S. back in the '90s, and now is found throughout the United States. It's transmitted by a number of different types of mosquitoes but specifically by one called Culex mosquitoes," says Dr. Pritt. "In many people, it can be completely asymptomatic or maybe cause just a mild illness. In some patients, it can cause swelling of the brain and spinal cord, and it can be very serious, if not fatal."
Watch: Dr. Bobbi Pritt talks about West Nile virus.
Journalists: Broadcast-quality sound bites are in the downloads at the end of the post. Please courtesy: "Bobbi Pritt, M.D./Microbiology/Mayo Clinic."
In less than 1% of infected people, the virus causes a serious nervous system, or neurological, infection. This may include inflammation of the brain, known as encephalitis, or of the membranes surrounding the brain and spinal cord, known as meningitis.
Signs and symptoms of neurological infections may include:
- High fever.
- Severe headache.
- Stiff neck.
- Disorientation or confusion.
- Coma.
- Tremors or muscle jerking.
- Seizures.
- Partial paralysis or muscle weakness.
- Vision loss.
- Numbness.
Symptoms usually last a few days. But signs and symptoms of encephalitis or meningitis can linger for weeks or months. Certain neurological effects, such as muscle weakness, can be permanent.
Seek medical attention right away if you have signs or symptoms of a serious infection, such as severe headaches, a stiff neck, disorientation or confusion. Hospitalization is usually necessary for a serious infection.
Diagnosis
"West Nile virus is diagnosed in the laboratory using serology tests to detect the patient's immune response to the virus. Polymerase chain reaction, or PCR, can also be helpful early on in disease for detecting the virus's genetic material before an immune response is detectable," says Dr. Pritt. "We just started offering a highly sensitive West Nile virus PCR assay in my laboratory that can detect viral RNA from blood, serum, urine and cerebrospinal fluid, and we have been detecting positive cases every week."
Learn about Mayo Clinic Laboratories' West Nile virus test.
Prevention
No vaccines are available to prevent illness or infection.
"The best way to prevent West Nile virus disease is to avoid mosquito bites," says Dr. Pritt. "This can be done by staying indoors from dusk to dawn when biting mosquitos are most abundant and to always wear an insect repellent on exposed skin when outdoors."
To avoid mosquito bites:
- Use insect repellent with DEET, picaridin or oil of lemon eucalyptus.
- Wear permethrin-treated clothing while outdoors or in the woods.
- Empty standing water in outdoor areas, including pet bowls and rain barrels.
- Install screens in windows.
"It's hard to predict who's going to get the fatal disease and who won't, and, therefore, it's best to just prevent against mosquito bites in general, Dr. Pritt says.
Related stories:
- "Uptick in vector-borne illnesses in US and what it means to you."
- "Tick-borne infections and the complicated role of climate change."
- "Mayo Clinic Minute: How to ease the itch of mosquito bites."
For the safety of its patients, staff and visitors, Mayo Clinic has strict masking policies in place. Anyone shown without a mask was either recorded prior to COVID-19 or recorded in a nonpatient care area where social distancing and other safety protocols were followed.
Related Articles