-
Weekend Wellness: Will diverticulitis come back?
DEAR MAYO CLINIC:
I was recently diagnosed with diverticulitis.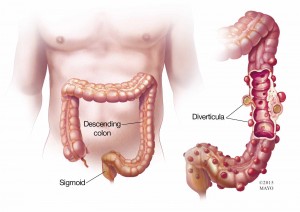 It was treated and the symptoms went away, but I’m wondering what could have caused it? I’m a 52-year-old man with no other medical problems. Am I at an increased risk for developing diverticulitis again since I’ve had it before?
It was treated and the symptoms went away, but I’m wondering what could have caused it? I’m a 52-year-old man with no other medical problems. Am I at an increased risk for developing diverticulitis again since I’ve had it before?
ANSWER:
Diverticulitis happens when small pockets that develop in the lining of your digestive tract become inflamed or infected. Treatment for diverticulitis focuses on eliminating the infection or inflammation, but it does not get rid of the pockets. Because those pockets remain, there is some risk you could get diverticulitis again, yet that risk is less than 10 to 15 percent. In some cases, making certain lifestyle changes may help lower the risk.
As we age, it is common for small, bulging pockets to form due to pressure at weak spots in the digestive tract lining. The pockets are called diverticula. They most often occur in the large intestine, or colon. By themselves, these pockets do not typically cause any problems or lead to symptoms.
When diverticulitis develops and one or more of the pockets becomes infected or inflamed, that can result in significant symptoms. These may include persistent and severe abdominal pain, nausea, vomiting and constipation. In some cases, diverticulitis can result in diarrhea, but that is less common than constipation.
Several factors may play a role in raising your risk for diverticulitis. As mentioned earlier, digestive tract pockets become more common with age. Diverticulitis most often affects people older than 40. Men tend to develop the condition more often than women. Obesity can increase the risk of diverticulitis, too, as can smoking. A lack of regular exercise may contribute to diverticulitis, as well.
Although you can’t do anything about your age or being male, you can take steps to lower your risk in other areas. Exercising regularly, losing weight if you need to and avoiding smoking can all help.
The specific role that diet plays in preventing diverticulitis is unclear. In the past, some doctors recommended that people who had diverticula not eat seeds and nuts, including foods with small seeds, such as tomatoes, cucumbers and strawberries. It was thought that these tiny food particles could lodge in the pockets and cause diverticulitis. But there is no scientific evidence of that, and doctors no longer recommend these foods be avoided.
Some experts have advocated eating a high-fiber diet — which may include nuts and seeds — to lower the risk of diverticulitis. A high-fiber diet on its own, however, has not been shown to prevent diverticulitis.
At this time, it appears that no specific foods trigger diverticulitis, and there is no special diet recommended to prevent it, either. So before you make any big changes to your diet in an effort to lower your risk of developing diverticulitis again, talk with your doctor about your individual needs to decide what is best for you. In many cases, eating a variety of well-balanced and nutritious foods along with plenty of fluids are good choices.
You should also review with your doctor any medications you are taking. Several drugs are associated with an increased risk of diverticulitis, including steroids, opiates and nonsteroidal anti-inflammatory drugs, such as ibuprofen and naproxen. Your doctor can help you determine if you may need to change any of your medications based on your history of diverticulitis.
If you have symptoms of diverticulitis again, contact your doctor right away. He or she will likely suggest testing to confirm the diagnosis before prescribing treatment. If it is confirmed, treatment would consist of a clear-liquid diet for a few days along with antibiotics. You would then return to a more normal diet as your symptoms improve. — John Cangemi, M.D., Gastroenterology, Mayo Clinic, Jacksonville, Fla.